Latest Articles
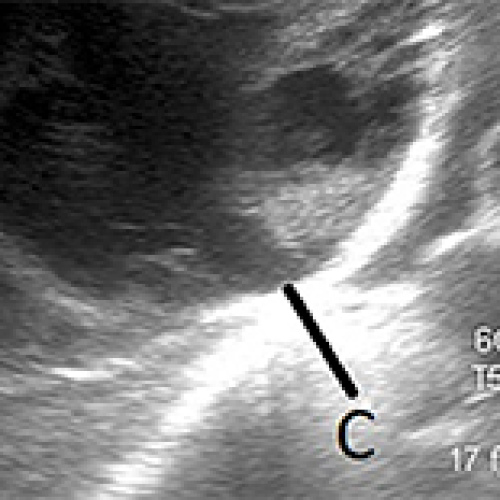
27 Apr 2024 : Case report 
A Rare Autochthonous Case of Hepatic Hydatid Cyst in the Non-Endemic Region of Taiwan
Mao-Yuan Chen, Tsung-Lin Chen
DOI: 10.12659/AJCR.943687
Am J Case Rep 2024; 25:e943687
27 Apr 2024 :
Case report 
A Rare Autochthonous Case of Hepatic Hydatid Cyst in the Non-Endemic Region of Taiwan
Mao-Yuan Chen, Tsung-Lin Chen
DOI: 10.12659/AJCR.943687
Am J Case Rep 2024; 25:e943687
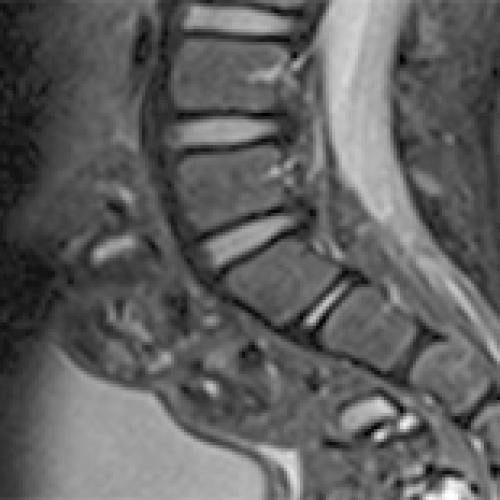
26 Apr 2024 : Case report 
Early Diagnosis and Successful Empirical Treatment of L1-L2 Spondylodiscitis in a 21-Month-Old Girl: A Case Report
Shaikha Mahmood Janahi, Walaa Abdulaziz Ashoor
DOI: 10.12659/AJCR.943010
Am J Case Rep 2024; 25:e943010
26 Apr 2024 : Case report 
Early Diagnosis and Successful Empirical Treatment of L1-L2 Spondylodiscitis in a 21-Month-Old Girl: A Case Report
Shaikha Mahmood Janahi, Walaa Abdulaziz Ashoor
DOI: 10.12659/AJCR.943010
Am J Case Rep 2024; 25:e943010
26 Apr 2024 : Case report 
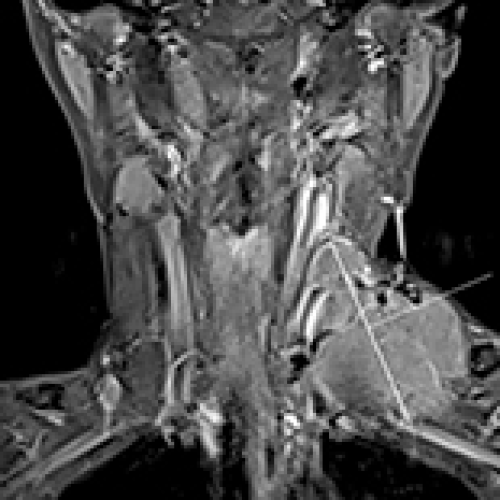
Castleman Disease Presenting in the Neck: A Report of 3 Cases and a Literature Review
Peng Jiang, Zheng-hui Huang
DOI: 10.12659/AJCR.943214
Am J Case Rep 2024; 25:e943214
26 Apr 2024 : Case report 
Castleman Disease Presenting in the Neck: A Report of 3 Cases and a Literature Review
Peng Jiang, Zheng-hui Huang
DOI: 10.12659/AJCR.943214
Am J Case Rep 2024; 25:e943214
25 Apr 2024 : Case report 
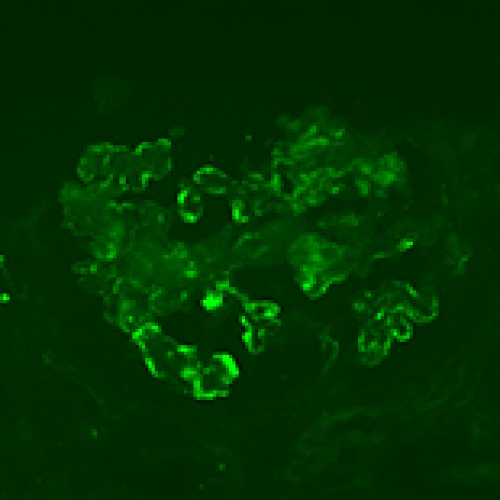
Simultaneous Occurrence of Collagen Type III Glomerulopathy and Immunoglobulin A Nephropathy: A Rare Case Report
Noura M. Aloudah ![]() , Samiah Hussain Moalwi
, Samiah Hussain Moalwi ![]()
DOI: 10.12659/AJCR.942770
Am J Case Rep 2024; 25:e942770
25 Apr 2024 : Case report 
Simultaneous Occurrence of Collagen Type III Glomerulopathy and Immunoglobulin A Nephropathy: A Rare Case Report
Noura M. Aloudah ![]() , Samiah Hussain Moalwi
, Samiah Hussain Moalwi ![]()
DOI: 10.12659/AJCR.942770
Am J Case Rep 2024; 25:e942770
25 Apr 2024 : Case report 
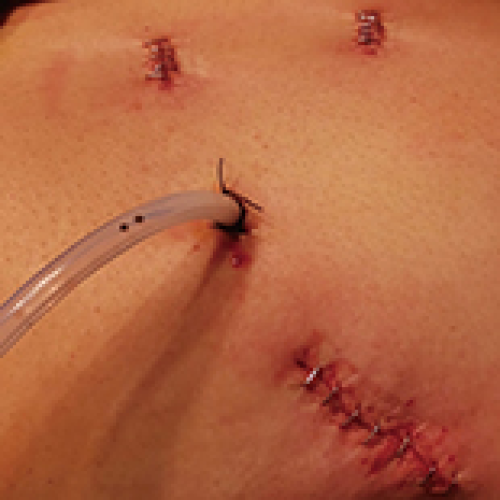
Management of Nontraumatic Spontaneous Renal Hemorrhage (Wünderlich Syndrome) through Robotic-Assisted Laparoscopic Nephrectomy: A Case Series
Boju Tao, Haoxun Zhang
DOI: 10.12659/AJCR.942826
Am J Case Rep 2024; 25:e942826
25 Apr 2024 : Case report 
Management of Nontraumatic Spontaneous Renal Hemorrhage (Wünderlich Syndrome) through Robotic-Assisted Laparoscopic Nephrectomy: A Case Series
Boju Tao, Haoxun Zhang
DOI: 10.12659/AJCR.942826
Am J Case Rep 2024; 25:e942826

24 Apr 2024 : Case report 
Pathogenic Potential of a PCK1 Gene Variant in Cytosolic PEPCK Deficiency: A Compelling Case Study
Monika Duś-Żuchowska ![]() , Hanna Nowak
, Hanna Nowak ![]()
DOI: 10.12659/AJCR.943118
Am J Case Rep 2024; 25:e943118

24 Apr 2024 : Case report 
Pathogenic Potential of a PCK1 Gene Variant in Cytosolic PEPCK Deficiency: A Compelling Case Study
Monika Duś-Żuchowska ![]() , Hanna Nowak
, Hanna Nowak ![]()
DOI: 10.12659/AJCR.943118
Am J Case Rep 2024; 25:e943118

24 Apr 2024 : Case report 
Laparoscopic Sleeve Gastrectomy with Staple-Line Oversewing in a Patient with Factor XI Deficiency: A Case Report
Lorenza Beomonte Zobel ![]() , Sirvjo Dhimolea
, Sirvjo Dhimolea
DOI: 10.12659/AJCR.942824
Am J Case Rep 2024; 25:e942824

24 Apr 2024 : Case report 
Laparoscopic Sleeve Gastrectomy with Staple-Line Oversewing in a Patient with Factor XI Deficiency: A Case Report
Lorenza Beomonte Zobel ![]() , Sirvjo Dhimolea
, Sirvjo Dhimolea
DOI: 10.12659/AJCR.942824
Am J Case Rep 2024; 25:e942824

23 Apr 2024 : Case report 
Eosinophilic Pleural Effusion Secondary to Trichinella spiralis Infection in a Patient with Systemic Sclerosis: A Case Report
Mădălina Ștefania Vulcan ![]() , Andrei-Daniel Dragne
, Andrei-Daniel Dragne ![]()
DOI: 10.12659/AJCR.943420
Am J Case Rep 2024; 25:e943420

23 Apr 2024 : Case report 
Eosinophilic Pleural Effusion Secondary to Trichinella spiralis Infection in a Patient with Systemic Sclerosis: A Case Report
Mădălina Ștefania Vulcan ![]() , Andrei-Daniel Dragne
, Andrei-Daniel Dragne ![]()
DOI: 10.12659/AJCR.943420
Am J Case Rep 2024; 25:e943420
23 Apr 2024 : Case report 
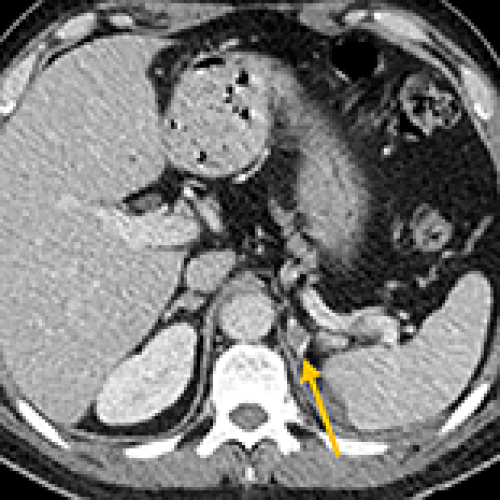
Cardiac and Intramuscular Metastases Following Nephroureterectomy for Metachronous Urothelial Carcinoma
DOI: 10.12659/AJCR.942864
Am J Case Rep 2024; 25:e942864
23 Apr 2024 : Case report 
Cardiac and Intramuscular Metastases Following Nephroureterectomy for Metachronous Urothelial Carcinoma
DOI: 10.12659/AJCR.942864
Am J Case Rep 2024; 25:e942864
22 Apr 2024 : Case report 
Unveiling the Temporal Aspect of MRI Tattoo Reactions: A Prospective Evaluation of a Newly-Acquired Tattoo with Multiple MRI Scans
Kasper Køhler Alsing ![]() , Helle Hjorth Johannesen
, Helle Hjorth Johannesen ![]()
DOI: 10.12659/AJCR.943411
Am J Case Rep 2024; 25:e943411
22 Apr 2024 : Case report 
Unveiling the Temporal Aspect of MRI Tattoo Reactions: A Prospective Evaluation of a Newly-Acquired Tattoo with Multiple MRI Scans
Kasper Køhler Alsing ![]() , Helle Hjorth Johannesen
, Helle Hjorth Johannesen ![]()
DOI: 10.12659/AJCR.943411
Am J Case Rep 2024; 25:e943411
22 Apr 2024 : Case report 
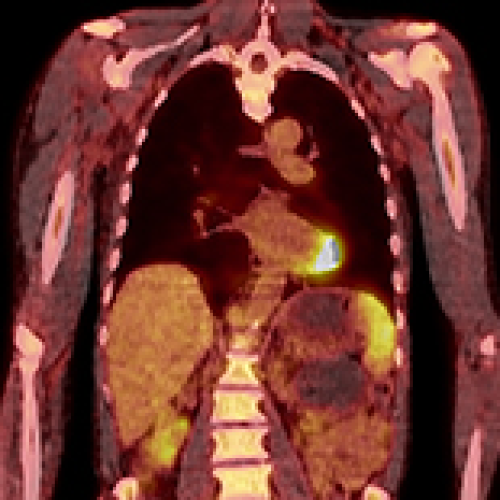
Recurrent Marginal Zone Lymphoma with Bone Marrow Involvement Detected by ¹⁸F-FDG PET/CT and Biopsy: A Diagnostic Challenge
Yeong-Shin Hsiao, Shu-Chane Shen
DOI: 10.12659/AJCR.943275
Am J Case Rep 2024; 25:e943275
22 Apr 2024 : Case report 
Recurrent Marginal Zone Lymphoma with Bone Marrow Involvement Detected by ¹⁸F-FDG PET/CT and Biopsy: A Diagnostic Challenge
Yeong-Shin Hsiao, Shu-Chane Shen
DOI: 10.12659/AJCR.943275
Am J Case Rep 2024; 25:e943275
21 Apr 2024 : Case report 
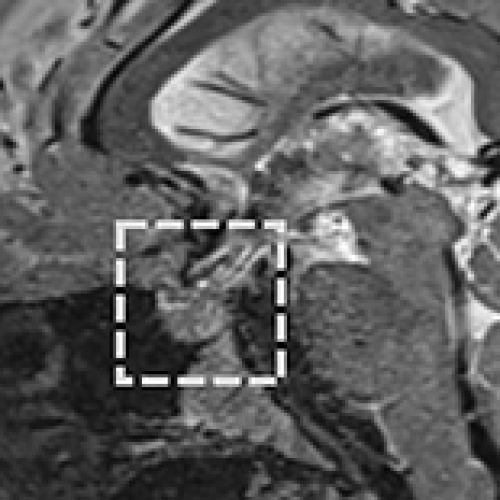
Successful Treatment of Lithium-Induced Nephrogenic Diabetes Insipidus with Celecoxib: A Promising Therapeutic Option
Ryunosuke Hashikawa, Hiroyuki Yamada
DOI: 10.12659/AJCR.943244
Am J Case Rep 2024; 25:e943244
21 Apr 2024 : Case report 
Successful Treatment of Lithium-Induced Nephrogenic Diabetes Insipidus with Celecoxib: A Promising Therapeutic Option
Ryunosuke Hashikawa, Hiroyuki Yamada
DOI: 10.12659/AJCR.943244
Am J Case Rep 2024; 25:e943244
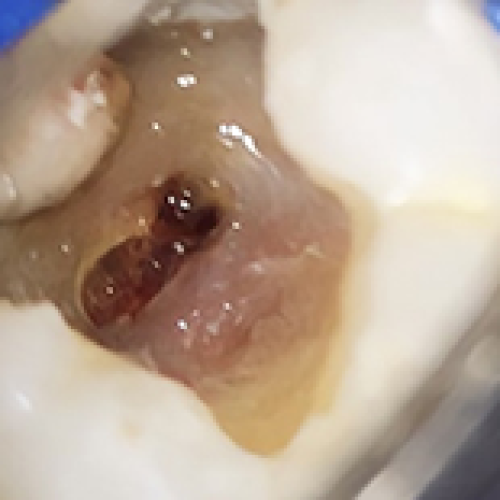
20 Apr 2024 : Case report 
Successful Healing of Periapical Pathology with Partial Pulpotomy in a Mature Permanent Molar: A Case Report
DOI: 10.12659/AJCR.942937
Am J Case Rep 2024; 25:e942937
20 Apr 2024 : Case report 
Successful Healing of Periapical Pathology with Partial Pulpotomy in a Mature Permanent Molar: A Case Report
DOI: 10.12659/AJCR.942937
Am J Case Rep 2024; 25:e942937
In Press
17 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943070
17 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943370
18 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943803
18 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943467
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250








