02 September 2020: Articles 
Diffuse Intrasinusoidal Hepatic Metastasis from Breast Cancer Presenting as Liver Failure: Effective and Rapid Treatment with Weekly Low-Dose Adriamycin
Challenging differential diagnosis, Unusual setting of medical care
Thanh-Phuong N. Afiat1BDEF*, Timothy N. Hembree12BDEF, Erin A. Dean3BDEF, Cyrillo Araujo24DEF, Luis R. Pena5DEF, Marilin Rosa6DE, Hyo S. Han27DEF, Kaitlin Hendrix8E, Asha Ramsakal12EFDOI: 10.12659/AJCR.924141
Am J Case Rep 2020; 21:e924141
Abstract
BACKGROUND: Hepatic metastasis is well known in breast cancer. Approximately 12–20% of breast cancer patients will develop liver metastasis, which usually presents as discrete mass lesions. Rarely, metastatic spread can be so diffuse that it is unidentifiable on imaging but can progress to fulminant hepatic failure. Our case report suggests that clinicians need to have a high index of suspicion when patients present with rapidly decompensating liver failure in the absence of discrete radiologic hepatic lesions, and that weekly Adriamycin should be considered as a first-line therapeutic option.
CASE REPORT: A 28-year-old African American woman with a history of locally advanced estrogen receptor-positive, progesterone receptor-negative, and HER2-negative breast cancer presented with right upper quadrant abdominal pain and bilateral lower extremity swelling. She had been treated 3 years prior with neoadjuvant Adriamycin/cyclophosphamide – Taxol, bilateral mastectomies, radiation therapy, and tamoxifen. Diagnostic imaging revealed massive hepatomegaly and extensive areas of liver ischemia/necrosis without discrete masses or arterial/venous thrombosis. Biopsy of the liver revealed metastatic carcinoma diffusely infiltrating the hepatic sinusoids. Extensive work up for other etiologies of liver disease was negative. The patient’s liver function quickly decompensated over several days. She was treated with weekly single-agent low-dose Adriamycin, and this resulted in successful reversal of her liver function tests back to baseline.
CONCLUSIONS: In addition to having a high index of suspicion for diffuse intrasinusoidal hepatic metastasis, physicians should consider weekly low-dose Adriamycin as a first-line therapeutic option for patients with progressive liver failure and biopsy-confirmed metastatic carcinoma diffusely infiltrating the hepatic sinusoids.
Keywords: Breast Neoplasms, Liver, Liver Failure, Acute, Pregnancy, Liver failure, Liver Neoplasms, tamoxifen
Background
Metastatic disease can occur many years after the initial diagnosis and treatment of early-stage breast cancer. It has been estimated that approximately 12–20% of breast cancer patients will develop liver metastasis [1]. Hepatic metastasis from breast cancer usually presents as discrete mass lesions readily distinguished on radiographic images. Rarely, meta-static spread can be so diffuse that it is unidentifiable on imaging [2]. When metastatic breast cancer infiltrates the hepatic sinusoids, patients are first diagnosed clinically after presenting with symptoms of hepatitis and rapidly progressive liver failure. Fulminant hepatic failure resulting from diffuse intra-sinusoidal metastatic disease from breast cancer is an uncommon but recognized presentation of hepatic involvement [3]. According to Allison [4], pathologically, “the pattern is consistently described as causing a grossly enlarged liver, usually with a well-preserved shape and general architecture. Pale, sharply demarcated regions and areas of infarction are present. The neoplastic cells infiltrate the hepatic sinusoids and can invade branches of the hepatic and portal veins. In some cases, a prominent desmoplastic response to the malignant cells occurs, and the appearance of the liver can mimic cirrhosis. Hepatocytes may be destroyed by pressure atrophy or vascular infarction, resulting in liver failure and a rapidly fatal course” [4]. This rare complication, as in our patient, often presents with rapid onset of ascites, and with marked elevation of bilirubin and hypoalbuminemia.
Breast cancer treatment in the setting of rapidly progressive liver failure represents a therapeutic challenge. Not only is the prognosis poor, but toxicity related to treatment can be unpredictable due to altered drug clearance. Bilirubin exceeding 5.0 mg/dL often is considered an absolute contraindication to the administration of chemotherapeutic agents dependent on hepatic metabolism. Weekly low-dose Adriamycin chemotherapy has previously been shown to minimize toxicity while maintaining dose intensity, and represents an alternative strategy for treatment of patients with hepatic impairment [5].
Case Report
A 28-year-old BRCA1/2-negative African American woman was being treated for clinical Stage III, T3N1M0, left breast cancer. The cancer was 90% estrogen receptor-positive, progesterone receptor-negative, and human epidermal growth factor receptor 2 (HER2)-negative by immunohistochemistry. She had no other significant past medical history or family history. She completed neoadjuvant chemotherapy with dose-dense Adriamycin/Cyclophosphamide×4 cycles (12/26/2016-2/6/2016) and Taxol×4 cycles (2/27/2017-4/10/2017), followed by bilateral mastectomies with left axillary lymph node dissection, right latissimus/implant reconstruction, and left tissue-expander placement on 5/26/2017. Surgical pathology noted residual isolated foci of invasive ductal carcinoma, comprising approximately 1% of a 6–7 cm tumor bed, presence of lymphovascular space invasion, and 1 lymph node with isolated tumor cells with chemotherapy-induced changes (0/18). She completed radiation therapy to the chest wall following surgery on 8/21/2017. Adjuvant endocrine therapy was recommended, including ovarian function suppression with monthly Goserelin and aromatase inhibitors, but she could not tolerate the Goserelin injections. Therefore, further tamoxifen was recommended, and she was doing well until February of 2019, when she notified the clinical team that she was pregnant, with a gestational age of 8 weeks. Tamoxifen was hence discontinued. Two weeks after cessation of tamoxifen, she was admitted to an outside hospital in March of 2019 with complaints of right upper quadrant (RUQ) abdominal pain, abdominal distention, bilateral lower extremity edema, and nausea and vomiting. Labs were remarkable for AST 208 U/L, ALT 49 U/L, ALKP 167 U/L, total bilirubin 1.1 mg/dL, and albumin 3.0 g/dL. A limited abdominal ultrasound showed hepatomegaly and possible acalculous cholecystitis. An early dating sonogram confirmed an intrauterine pregnancy of 10 weeks and 5 days. She then underwent a laparoscopy for possible cholecystectomy. During the procedure, a large cirrhotic-appearing liver with areas of necrosis was noted, and the procedure was aborted. Subsequent CT of the abdomen and pelvis revealed a large, partially necrotic mass occupying the entire right hepatic lobe measuring 17×14×20 cm, invading and occluding the posterior branch of the right portal vein and exerting a mass effect on the intrahepatic inferior vena cava (IVC) to near complete occlusion. There was also necrotic nodularity in the mesentery adjacent to the inferior liver tip, with invasion of the liver parenchyma. Extensive osseous metastatic disease was also noted. Intraoperative biopsy of the liver was taken and sent for intraoperative examination, which showed metastatic carcinoma. Microscopically, the entire available tissue was composed of nests of neoplastic cells diffusely infiltrating the hepatic sinusoids and without frank infiltration of the liver parenchyma (Figure 1). The hepatic architecture was disrupted due to tumor compression of the hepatocytes with areas of hepatocyte atrophy and necrosis as well as desmoplasia around some of the involved sinusoids. Immunostaining for CD31, an endothelial marker, was performed, and this highlighted the intrasinusoidal location of the tumor (Figure 2), which was also confirmed by trichrome special stain (Figure 3). Additional immunostains were performed to confirm the primary site of origin. The tumor was positive for GATA-3, estrogen receptor, and CK-7, and negative for CK-20, progesterone receptor, and HER2. Based on the clinical history of estrogen receptor-positive breast carcinoma and the immunohistochemistry results, the final diagnosis of metastatic breast carcinoma was rendered. The patient was discharged to her home with instructions to follow up with her oncologist and gynecologist. However, she presented a few days later to our ER due to persistent abdominal pain.
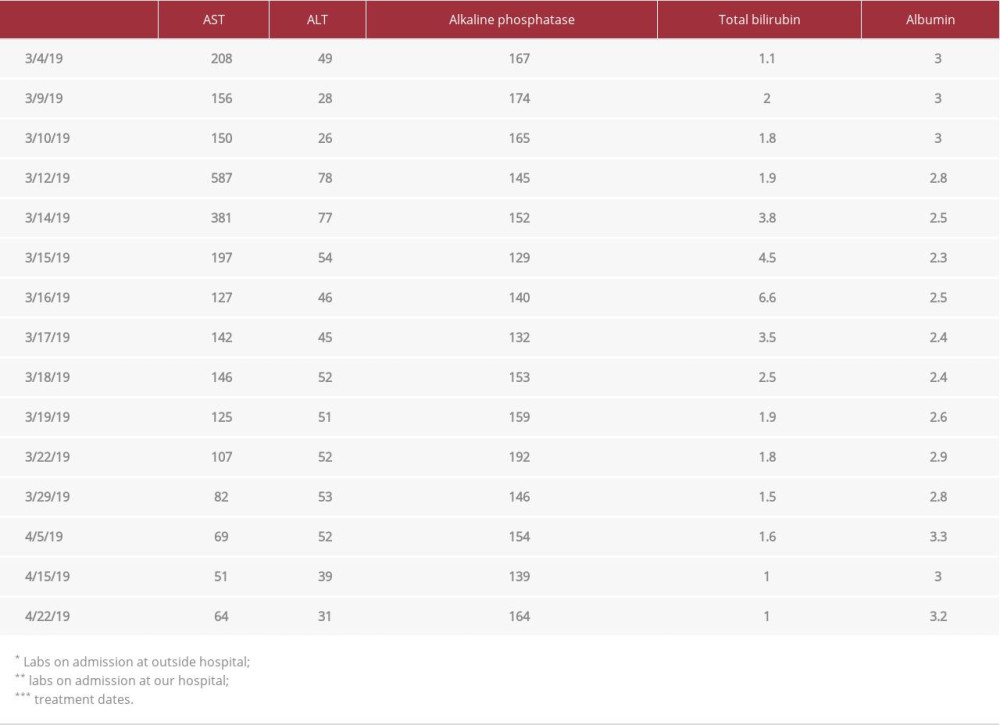
At our facility, in addition to the identical persistent symptoms treated at the outside hospital, she complained of new left-side rib pain in the area of new osseous metastases. Physical exam noted a distended abdomen with tenderness to palpation in the right upper quadrant and epigastric area, with hepatomegaly and 2+pitting edema in the bilateral lower extremities. MRI of the abdomen showed liver edema and necrosis (Figure 4). Labs were significant for AST 156 U/L, ALT 28 U/L, ALKP 174 U/L, total bilirubin 2.0 mg/dL, INR 1.6, Alb 3.0 g/dL, LDH 953, and hemoglobin 8.4 g/dL. The patient electively underwent termination of the pregnancy. Over the next 3 days, the patient had rapid progression of her liver failure with increasing AST (587 U/L), ALT (78 U/L), ALKP (145 U/L), total bilirubin (1.9 mg/dL), and Alb (2.8 g/dL) (Table 1). She became febrile with Tmax 38.6°C, tachycardic with maximum heartrate of 149, and more lethargic with persistent pain. She also complained of shortness of breath. She was started on empiric cefepime. A CT chest angiogram was performed, which ruled out pulmonary embolism. Bilateral patchy ground-glass densities were identified and early lung metastasis could not be ruled out. An abdominal CT was obtained, which demonstrated massive hepatomegaly with enlarging infarcts mostly in the peripheral right lobe, with focal capsular disruption, and compression of the left portal vein and IVC (Figure 5). Liver ultrasound was negative for thrombus, with patent vasculature and appropriately directed flow. There was portal pulsatility and loss of hepatic vein phasicity consistent with compression of the IVC. Viral hepatitis serologies, acetaminophen levels, and autoimmune and infectious work up were all negative.
Given the patient’s worsening medical condition, goals of care were discussed, and the patient and her family wished to continue aggressive care. The case was thoroughly reviewed by the breast cancer tumor board and, ultimately, the decision was made to give palliative weekly low-dose Adriamycin. Within 3 days following the first cycle of Adriamycin (20 mg/m2 IV), her bilirubin had decreased to 1.9 mg/dL, AST to 125 U/L, ALT to 51 U/L, and ALKP to 159 U/L.
After 5 cycles of this regimen, the patient’s symptoms resolved, her total bilirubin level normalized, and her performance status returned to baseline. A restaging CT scan of the abdomen showed improved hepatomegaly and less compression of the intrahepatic IVC, with more organized hypo-enhancement of the liver, indicative of an improved infiltrative process with treatment response (Figure 6). Labs associated with poor liver function improved over time (Figure 7, Table 1). The patient was switched to monthly liposomal doxorubicin which she continued until November of 2019 with stable disease. However, due to progressive bone metastatic disease, her therapy was changed to abemaciclib and fulvestrant in December of 2019.
Discussion
This case illustrates the occurrence of a rare, aggressive form of diffuse intrahepatic sinusoidal metastatic breast cancer, in a pregnant patient presenting with acute liver failure, that was effectively and rapidly treated with weekly low-dose Adriamycin.
The severe deterioration of liver function had features typical of sinusoidal obstructive syndrome (SOS). The patient had significant hepatomegaly associated with right upper quadrant pain, jaundice, and ascites. Evidence of compression of the intrahepatic IVC was present, which has also been described as an etiology for SOS [6]. Although the level of elevation of liver enzymes and bilirubin can vary significantly depending on the liver area affected, her labs were consistent with her presentation. Liver ischemic injury was supported by LDH elevation. She had multiple small subsegmental infarcts mostly in the periphery of the right hepatic lobe, which have been seen in SOS due to tumor infiltration [7]. SOS is a complex pathologic entity of multifactorial etiology. In the present case, it was likely due to decreased hepatic venous outflow caused by liver congestion from tumor infiltration and IVC compression/stenosis.
The patient’s quick response to chemotherapy suggests that improvement of her liver failure was due to rapid reduction of tumor infiltration in the sinusoidal spaces, resulting in improved blood flow and decreased liver congestion.
The choice of chemotherapy agent for our patient was evidence based. Weekly Adriamycin has previously been shown to be efficacious in refractory advanced breast cancer. In a small randomized study involving 43 patients with breast cancer who had failed cyclophosphamide, methotrexate, and 5-fluorouriacil (CMF regimen), 2 weekly dosed anthracyclines were compared. Weekly Adriamycin with median cumulative dose of 240 mg/m2 (range 160–860) led to a complete-plus-partial response rate of 38%, a median duration of response of 7 months, and median survival of 11 months [8]. Our patient had a partial response to her therapies and improvement in quality of life.
Conclusions
Although hepatic metastasis is well known in breast cancer, diffuse intrasinusoidal hepatic metastasis is a rare form of metastatic disease. Clinicians need to have a high index of suspicion in breast cancer patients who present with rapidly decompensating liver failure and absence of discrete radiologic hepatic lesions. Additionally, in patients with progressive liver failure and biopsy-confirmed metastatic carcinoma diffusely infiltrating the hepatic sinusoids, weekly Adriamycin should be considered as a first-line therapeutic option.
Figures
References:
1.. Polistina F, Costantin G, Febbraro A, Aggressive treatment for hepatic metastases from breast cancer: Results from a single center: World J Surg, 2013; 37(6); 1322-32
2.. Hanamornroongruag S, Sangchay N, Acute liver failure associated with diffuse liver infiltration by metastatic breast carcinoma: A case report: Oncol Lett, 2013; 5; 1250-52
3.. Jen W, Chee Y, Khor L, Diffuse intrasinusoidal hepatic metastasis from occult breast carcinoma presenting as thrombotic microangiopathy: A case report and literature review: J Hematol, 2015; 4(4); 238-41
4.. Allison KH, Fligner CL, Parks WT, Radiographically occult, diffuse intrasinusoidal hepatic metastases from primary breast carcinomas: A clinicopathologic study of 3 autopsy cases: Arch Pathol Lab Med, 2004; 128(12); 1418-23
5.. Gurevich I, Akerley W, Treatment of the jaundiced patient with breast carcinoma: Case report and alternate therapeutic strategies: Cancer, 2001; 91(4); 660-63
6.. Bat-Erdene B, Orgoi S, Sandag E, Inferior vena cava stenosis-induced sinusoidal obstructive syndrome after living donor liver transplantation: Korean J Hepatobiliary Pancreat Surg, 2016; 20(3); 133-36
7.. : Clinical and Research Information on Drug-Induced Liver Injury [Internet], 2019, Bethesda (MD), National Institute of Diabetes and Digestive and Kidney Diseases -[Cited 2020 March 1]. Available from: .https://www.ncbi.nlm.nih.gov/books/NBK548032/
8.. Gasparini G, Dal Fior S, Panizzoni GA, Weekly epirubicin versus doxorubicin as second line therapy in advanced breast cancer. A randomized clinical trial: Am J Clin Oncol, 1991; 14(1); 38-44
Figures
In Press
14 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942770
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943214
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943010
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943687
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250