29 September 2020: Articles 
A 63-Year-Old Woman with SARS-CoV-2 Infection, Who Developed Severe COVID-19 Pneumonia and Was Supported with Convalescent Plasma Therapy
Unusual clinical course, Diagnostic / therapeutic accidents, Unusual setting of medical care, Unexpected drug reaction, Educational Purpose (only if useful for a systematic review or synthesis)
Anna Moniuszko-Malinowska1ABDEFG*, Piotr Czupryna1ABDEF, Barbara Boczkowska-Radziwon2BDEF, Tomasz Wasiluk2BDEF, Karol Borawski1BDE, Justyna Dunaj1BD, Magdalena Bujno2BD, Piotr Radziwon23BDE, Krzysztof Rutkowski4D, Sławomir Pancewicz1ABDEDOI: 10.12659/AJCR.927662
Am J Case Rep 2020; 21:e927662
Abstract
BACKGROUND: There is no evidence-based treatment for coronavirus disease 2019 (COVID-19). We report the case of a 63-year-old woman with SARS-CoV-2 infection who developed severe COVID-19 pneumonia and was treated with convalescent plasma.
CASE REPORT: A 63-year-old woman who presented with severe and prolonged course of COVID-19 disease (fever up to 39.4°C, persistent cough, and dyspnea) received a convalescent plasma transfusion, which led to complete recovery. The diagnosis was confirmed by RT-PCR testing using the CFX96 Real-Time System (Bio-Rad, USA) from nasopharyngeal swabs. In laboratory tests, an increase in acute-phase parameters was observed. Chest computed tomography (CT) showed abnormalities typical for COVID-19. On days 9 and 11 of the disease, she received the convalescent plasma prepared from a single plasmapheresis donation from a male donor. This male donor was qualified as a convalescent plasma donor according to Polish guidelines, which are compliant with European guidelines. He donated plasma at the Regional Centre for Transfusion Medicine in Białystok, Poland. The therapy with convalescent plasma led to clinical improvement and normalization of inflammatory parameters.
CONCLUSIONS: This report presents a case of severe COVID-19 pneumonia in a 63-year-old woman who was given supportive treatment with convalescent plasma. Ongoing clinical trials will determine whether convalescent plasma therapy is an effective treatment for SARS-CoV-2 infection.
Keywords: Antibodies, Complementary Therapies, COVID-19, Blood Component Transfusion, COVID-19, Coronavirus Infections, Follow-Up Studies, Pandemics, Pneumonia, Viral, RNA, Viral, Real-Time Polymerase Chain Reaction, Risk Assessment, severe acute respiratory syndrome
Background
The virus that causes coronavirus disease 2019 (COVID-19) is a beta coronavirus related to Severe Acute Respiratory Syndrome coronavirus (SARS-CoV-2). The new virus originated in China and since December 2019 it has spread throughout the world, causing over 21.8 million cases and 773 000 deaths, and the pandemic is still ongoing [1].
SARS-CoV-2 is transmitted by airborne droplets during coughing or sneezing and by close contact with infected individuals. The expression of angiotensin-converting enzyme-2 (ACE-2) receptor in the upper-respiratory tract correlates with the course of virus infection. SARS-CoV-2 utilizes ACE-2 as a receptor to enter host pneumocytes, which may explain its high infectivity. Moreover, comorbidities, such as diabetes, hypertension, heart diseases, and obesity, influence the course of COVID-19 [2].
The diagnosis of SARS-CoV-2 infections relies on PCR in samples taken from the upper- or lower-respiratory tract. The detection of antibodies against SARS-CoV-2 in blood may be useful. In symptomatic cases, chest CT plays a crucial role, as it reveals abnormalities, such as ground-glass lesions, patchy consolidations, alveolar exudates, and interlobular involvement, eventually indicating deterioration.
To date, no curative treatment has been found. There are no specific antiviral agents that target the novel virus, but other treatment methods, including plasma obtained from COVID-19 convalescents, are under investigation [3]. We report the case of a patient treated with plasma obtained from a convalescent patient, which led to a complete recovery.
Case Report
A 63-year-old woman with type 2 diabetes and hypertension, without any other risk factors, was referred to the Department of Infectious Diseases and Neuroinfections, Medical University of Białystok, Poland due to fever and cough. Her husband and daughter had been diagnosed with COVID-19. The sample taken from the patient in the Outpatient Department was positive for SARS-CoV-2. The diagnosis was made by reverse transcription-polymerase chain reaction (RT-PCR) testing using the CFX96 Real-Time System (Bio-Rad, USA) from nasopharyngeal swabs. Detection was made with the Seegene (CE-IVD) diagnostic kit. Three regions were detected: RdRP, N, and E.
There were no significant abnormalities on physical examination. Chest computed tomography (CT) on day 2 of admission revealed lesions suggestive of COVID-19 pneumonia (Figure 1A, 1B).
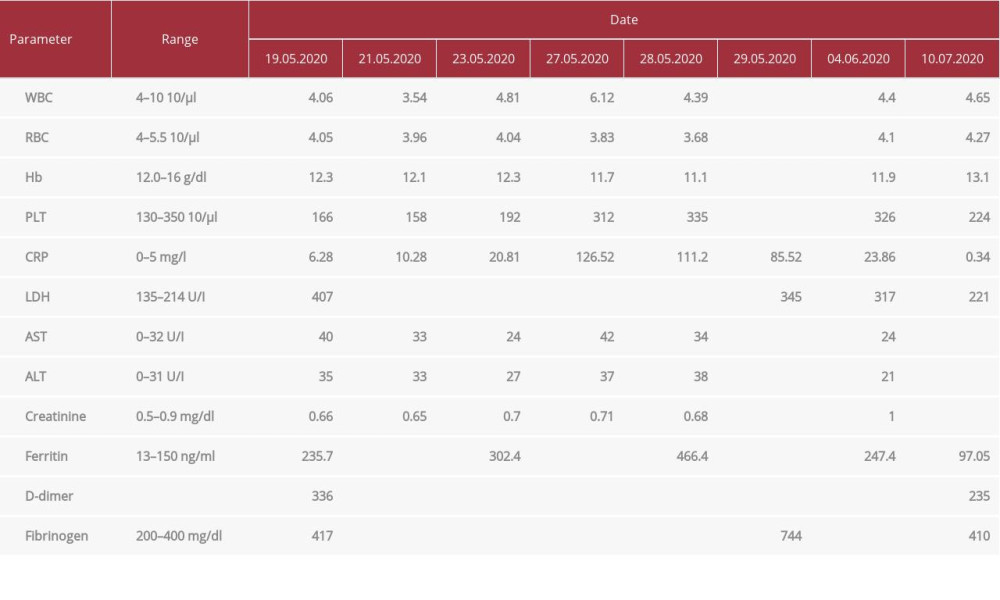
Despite 9 days of treatment with oral chloroquine (2×250 mg), the patient remained pyrexial up to 39.4°C and had persistent cough and dyspnea. There was an increase in acute-phase parameters (Table 1). A chest CT scan performed on day 8 showed progression of inflammatory changes (Figure 1C, 1D).
On days 9 and 11, she was given 250 mL of convalescent plasma intravenously, both prepared from a single plasmapheresis donation from a male donor. The donor had mild COVID-19 symptoms (1-day fever and loss of taste and smell). He was presumed healthy after 2 negative PCR test results. He was a suitable convalescent plasma donor according to Polish and European guidelines [4] and donated plasma at the Regional Centre for Transfusion Medicine in Białystok, Poland on 19.05.2020. After donation, the plasma was split into 3 equal portions. A pathogen reduction process involving the use of methylene blue (Macotronic, Macopharma, France) was applied to 2 portions, and the third was pathogen-reduced with amotosalen hydrochloride (Intercept, Cerus, USA). The plasma was frozen and kept at below −25°C until release. The plasma contained anti-SARS-CoV-2 antibodies: IgA >7 (positive >1.1), IgG – 8.37 (positive >1.1), IgG titer 1: 1500 (Euroimmun, USA) and IgG 57.60 AU/ml (positive >15 AU/ml) (DiaSorin, Italy).
The patient responded well to plasma therapy, with fever resolution, clinical improvement, and normalization of inflammatory parameters (Table 1). Subsequent PCR tests were negative 3 times. A change in anti-SARS-CoV-2 IgG antibodies titer was observed. Before infusion, the titer was 81.4 AU/ml (28.05). After the first infusion, the titer was 172 AU/ml (31.05). After the second infusion, the titer was 247 AU/ml (01.06) (DiaSorin, Italy). A repeat CT chest (day 20) showed regression of inflammatory changes (Figure 1E, 1F).
The patient was discharged on day 23 in good general condition. There were no treatment complications. At follow-up 6 weeks after discharge, she reported no symptoms, and all laboratory parameters were within normal ranges (Table 1).
Discussion
The quest for COVID-19 treatment continues. Thus far, there is not enough data to support the effectiveness of any particular treatment. Therefore, all data on various COVID-19 treatments are valuable.
There have been very few reports on the usefulness of convalescent plasma transfusions to treat COVID-19. They included a few case series, but no clinical trials. Their outcomes were encouraging, as improvement was observed in all patients treated with convalescent plasma, despite a severe course of the disease [5,6]. Convalescent plasma can lead to direct neutralization of the virus, modification of an overactive immune system (cytokine storm, Th1/Th17 ratio, complement activation), and a hypercoagulable state [7].
In 2015 Mair-Jenkins et al. reported that convalescent plasma transfusion may be beneficial for patients with viral severe acute respiratory infections. A meta-analysis of 32 studies on SARS coronavirus infections and severe influenza proved that transfusion of convalescent plasma had a clinically relevant impact in reducing the rate of mortality and viral load in these patients [8].
Studies performed during ongoing coronavirus pandemics confirm that patients with a severe infection can benefit from convalescent plasma transfusion and that the risk of adverse effects of such therapy is rather low [4,6,9–11]. The most common adverse reactions are transfusion-related events, involving rigors, fever, anaphylaxis, transfusion-related acute lung injury, circulatory overload, and hemolysis.
Therapy seems to be more effective if implemented during first 2 weeks after the onset of symptoms. Therefore, the optimal timing of administering convalescent plasma on COVID-19 needs to be carefully considered [12].
Our report confirms the beneficial effects of convalescent plasma in a patient with severe COVID-19 disease with complete resolution of symptoms and an increase in serum antibody titers after each transfusion and no adverse effects.
Convalescent plasma transfusion is one of the supportive treatment options for COVID-19. Ongoing clinical trials [13] may generate robust data on this promising treatment modality.
Conclusions
This report presents a case of severe COVID-19 pneumonia in a 63-year-old woman who was given supportive treatment with convalescent plasma. The results of ongoing controlled clinical trials are awaited to determine whether convalescent plasma therapy is an effective treatment for SARS-CoV-2 infection.
References:
2.. Zhou P, Yang YL, Wang XG, A pneumonia outbreak associated with a new coronavirus of probable bat origin: Nature, 2020; 579; 270-73
3.. Lu H, Drug treatment options for the 2019-new coronavirus (2019-nCoV): Biosci Trends, 2020; 14; 69-71
4.. , An EU programme of COVID-19 convalescent plasma collection and transfusion Guidance on collection, testing, processing, storage, distribution and monitored use: Ref. Ares, 2020 3256185–23/06/2020, https://ec.europa.eu/health/sites/health/files/blood_tissues_organs/docs/guidance_plasma_covid19_en.pdf
5.. Shen Ch, Wang Z, Zhao F, Treatment of 5 critically ill patients with COVID-19 with convalescent plasma: JAMA, 2020; 323(16); 1582-89
6.. Duan K, Liu B, Li C, Effectiveness of convalescent plasma therapy in severe COVID-19 patients: PNAS, 2020; 117(17); 9490-96
7.. Rojas M, Rodríguez Y, Monsalve DM, Convalescent plasma in Covid-19: Possible mechanisms of action: Autoimmun Rev, 2020; 19(7); 102554
8.. Mair-Jenkins J, Saavedra-Campos M, Baillie JK, The effectiveness of convalescent plasma and hyperimmune immunoglobulin for the treatment of severe acute respiratory infections of viral etiology: A systematic review and exploratory meta-analysis: J Infect Dis, 2015; 211(1); 80-90
9.. Chen L, Xiong J, Bao L, Shi Y, Convalescent plasma as a potential therapy for COVID-19: Lancet Infect Dis, 2020; 20(4); 398-400
10.. Valk SJ, Piechotta V, Chai KL, Convalescent plasma or hyperimmune immunoglobulin for people with COVID-19: A rapid review: Cochrane Database Syst Rev, 2020; 5(5); CD013600
11.. Harvala H, Mehew J, Robb ML, Convalescent plasma treatment for SARS-CoV-2 infection: Analysis of the first 436 donors in England, 22 April to 12 May 2020: Euro Surveill, 2020; 25(28); 2001260
12.. Zhao Q, He Y, Challenges of convalescent plasma therapy on COVID-19: J Clin Virol, 2020; 127; 104358
13.. Casadevall A, Joyner MJ, Pirofski LA, A randomized trial of convalescent plasma for COVID-19-potentially hopeful signals: JAMA, 2020; 324(5); 455-57
In Press
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943687
17 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943070
17 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943370
18 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943803
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250