20 September 2021: Articles 
Transcatheter Occlusion of a Giant Coronary Artery Fistula in a Neonate
Congenital defects / diseases
Shunsuke Yamada1BDEF, Mieko Aoki-Okazaki2AB, Manatomo Toyono1ADEF*DOI: 10.12659/AJCR.933079
Am J Case Rep 2021; 22:e933079
Abstract
BACKGROUND: Although large coronary artery fistulas are uncommon; they lead to substantial over-circulation in the pulmonary vascular beds and left heart system. Fistula occlusions are achieved via surgical or transcatheter technique; however, reports on successful outcomes of transcatheter treatment during the neonatal period are limited.
CASE REPORT: A female infant was born at the gestational age of 37 weeks with a birth weight of 2615 grams via normal vaginal delivery. Cardiac auscultation revealed a loud continuous murmur emanating from the fourth right intercostal space. A right coronary artery-to-right ventricle fistula was confirmed using transthoracic echocardiography. The newborn developed respiratory distress 3 days after birth and was administered continuous positive airway pressure to assist breathing. On day 8, the ventilator was used through tracheal intubation due to gradual worsening of dyspnea. A 6-mm Amplatzer Vascular Plug 4 (AGA Medical Corporation, Plymouth, MN) was chosen, as the minimum diameter of the coronary artery fistula was 5 mm. In view of the risk of myocardial ischemia with additional devices, the procedure was stopped despite persistent shunting. The newborn’s clinical condition significantly improved following the procedure and she was eventually weaned off ventilator support.
CONCLUSIONS: A self-expanding occlusion device was useful for relieving this life-threatening condition. Complete elimination of shunting is not always necessary, to avoid compromising myocardial circulation.
Keywords: Coronary Vessels, Fistula, Heart Ventricles, Infant, Newborn, Therapeutics, cardiac catheterization, Coronary Angiography, Coronary Artery Disease, Coronary Vessel Anomalies, Female, Humans, Infant
Background
Most coronary artery fistulas are small and asymptomatic. Large coronary artery fistulas uncommonly lead to substantial over-circulation in the pulmonary vascular beds and left heart system, potentially increasing the risk of myocardial ischemia, heart failure, and pulmonary hypertension [1]. The presence of congestive heart failure and/or distal coronary insufficiency warrants therapeutic interventions such as transcatheter occlusion or open surgical ligation on the coronary artery fistula [2,3]. Transcatheter occlusion of coronary artery fistulas is associated with good short-term procedural success rates and complication rates in selected patients [4]; however, reports on successful outcomes during the neonatal period are limited [2,5,6]. Here, we describe the transcatheter management of a neonate who developed congestive heart failure associated with a giant right coronary artery-to-right ventricle fistula.
Case Report
In a 28-year-old woman (gravida 1, para 1), with fetal cardiomegaly, was identified through routine scanning at the gestational age of 22 weeks. She was in good health without any maternal complications or high-risk factors. Further examination revealed an abnormal vessel originating from the ascending aorta and a dilated right ventricle in the fetus. The drainage site of the abnormal vessel was not identified; however, diastolic reversal in the aorta suggested a diagnosis of coronary artery-to-right ventricle fistula. The size of the abnormal vessel gradually increased during pregnancy. No interventions were performed after the identification of the anomaly because normal fetal growth was periodically confirmed.
A female infant was born at the gestational age of 37 weeks with a birth weight of 2615 g via normal vaginal delivery. On physical examination, her respiratory rate was 65 per min, apical rate 140 per min, and blood pressure 50/27 mmHg (normal reference ranges: respiratory rate 30 to 50 per min, apical rate 120 to 160 per min, and blood pressure 70/40 mmHg or greater, respectively). Cardiac auscultation revealed a loud continuous murmur emanating from the 4th right intercostal space.
Prenatal findings suggesting a right coronary artery-to-right ventricle fistula were confirmed after delivery using transthoracic echocardiography (Figure 1A–1D). A chest X-ray on the first day indicated increased pulmonary vascularity within the bilateral lung fields; therefore, a continuous intravenous infusion of phosphodiesterase-3 inhibitors (olprinone, 0.3 µg/kg/minute) was initiated. An electrocardiogram on the second day did not show ischemic change (Figure 2). The newborn developed respiratory distress 3 days after birth and was administered continuous positive airway pressure to assist breathing. On day 8, the ventilator was used through tracheal intubation due to gradual worsening of dyspnea. The plasma B-type natriuretic peptide level was 6753 pg/ml at the time. Enhanced computed tomography angiography exhibited a single stenotic site (neck) in the entire fistula.
A decision was made to percutaneously close the fistula; 22 days after birth, the procedure was performed under generalized anesthesia during which, unfractionated heparin was administered. As her bilateral femoral arteries were narrow, vascular access was via the common carotid artery using an introducer sheath to avoid prolonged attempts through the fem-oral artery; the approach was retrograde arterial loop. A soft-tipped stiff wire was advanced, followed by a 4-Fr catheter over the wire; selective coronary angiography was performed prior to the procedure to delineate the anatomy of the giant distal fistula (Figure 3A, 3B). Due to the tortuousness of the fistula requiring placement in a controlled fashion, and its high-flow communication, a self-expanding occlusion device was selected for closure. A 6-mm Amplatzer Vascular Plug 4 (AGA Medical Corporation, Plymouth, MN) was chosen, as the minimum diameter of the coronary artery fistula was 5 mm; great care was taken not to compromise circulation to the myocardium. The correct location of the device was confirmed through angiography before its release from the delivery cable. After deployment of the device, to verify the correct position and a possible residual flow across the target structure (Figure 3C, 3D), a repeat angiography was immediately performed. In view of the risk of myocardial ischemia with additional devices, the procedure was stopped despite persistent shunting. The newborn’s clinical condition significantly improved following the procedure and she was eventually weaned off ventilator support. After a 2-week hospital stay, she was discharged home with a prescription for aspirin (5 mg/kg/day). There was no occurrence of post-procedural myocardial infarction, vascular complications, or stroke.
During the 16-month follow-up period, she remained both stable and asymptomatic, with no evidence of myocardial infarction; the size of her right ventricle had normalized, and the B-type natriuretic peptide plasma level was 10.5 pg/mL. Although post-procedural angiography revealed a small persistent shunting, the mean pulmonary arterial and pulmonary capillary wedge pressures were not elevated (13 and 9 mmHg, respectively).
Discussion
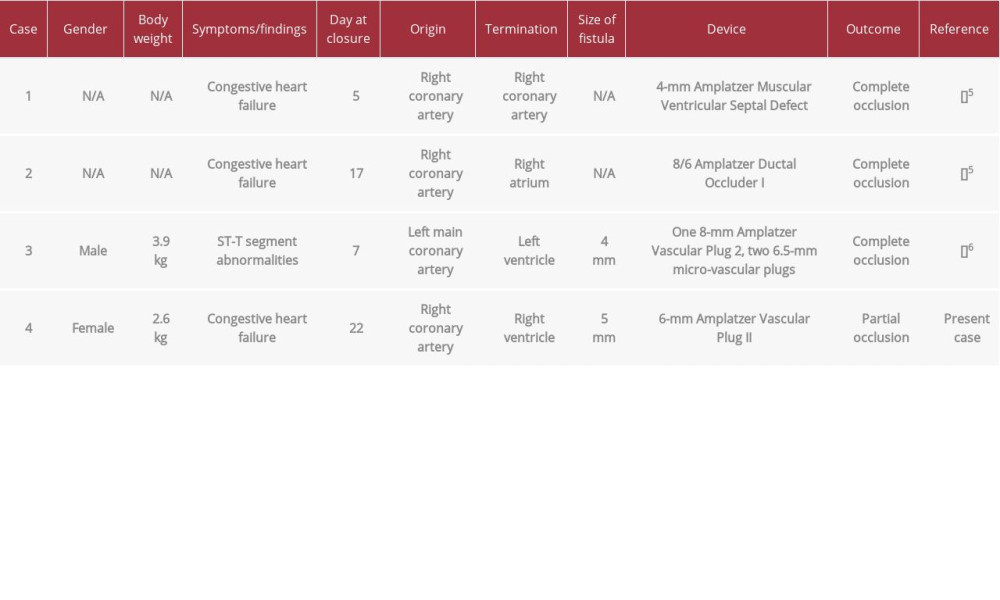
A coronary artery fistula is rarely large enough to exert a substantial effect on hemodynamics. For a fistula that is symptomatic, invasive treatment by transcatheter occlusion or surgical ligation is usually a reasonable choice, and both strategies show comparable results in long-term follow-up [7]. To date, reports on successful outcomes during the neonatal period have been limited (Table 1). According to the previous reports, the body weights of the patients who underwent transcatheter occlusion of coronary artery fistulas during the neonatal period ranged from 3.4 to 3.9 kg [2,5,6]; therefore, we would like to emphasize that our patient (2.6 kg) was the lightest. Even in a neonate with a body weight less than 3 kg, a fistula can be treated with transcatheter occlusion accessed via the common carotid artery. In addition, all neonatal cases were treated with self-expandable devices, leading to closure of the coronary artery fistulas.
Although right coronary artery-to-right ventricle shunting persisted after transcatheter therapy of the fistula in our case, post-procedural improvement was substantial. In a 21-year experience of transcatheter therapy of coronary artery fistula at the Mayo Clinic, 3 of 16 patients who had an acute persistent shunting of trivial grade showed an increase in residual flow during the follow-up period [4]. In a study of 15 years of transcatheter treatment at another institution, of the 9 patients who required re-intervention, the reason of re-intervention was persistent shunting only in 1, and those included myocardial ischemia, device embolization, and valve injury in the others [8]. Based on these experiences, it is quite possible that complete elimination of shunting is not always necessary. Closure of small-to-moderate coronary artery fistulas is recommended in the presence of symptoms of myocardial ischemia, threatening arrhythmia, unexplained ventricular dys-function, or left atrial hypertension [9]. No data have been reported on asymptomatic coronary artery fistulas to establish the maximum magnitude of shunting through a fistula that is considered harmless.
Transcatheter treatment is associated with a high incidence of adverse events in children [10]. Known complications of trans-catheter occlusion of coronary artery fistulas include residual shunt due to incomplete closure, myocardial ischemia due to closure of side branches of peripheral normal coronary artery, coil migration and embolization in the right ventricular system, transient ST changes on electrocardiograms, and atrioventricular block [7]. In addition, there is a significant risk of complication at the site of arterial puncture in infants weighing less than 4 kg [11]. The risk of complication is high in the first 6 months of life, and 0.23% of deaths are reported in neonates [12]. In contrast, in neonatal cardiac catheterization, low-birth-weight infants weighing less than 2.5 kg have significantly more minor complications than those weighing more than 2.5 kg, but there is no difference in the frequency of serious complications, according to 1 report [13]. The relationship between the number of years of experience of the operators and adverse events has been reported from the United States in a multicenter registry; the incidence of adverse events was significantly higher among operators with less than 5 years of experience [14].
In this case, the following conditions were met for transcatheter occlusion of the coronary artery fistula: (1) possible safe insertion of the catheter into the coronary artery fistula, (2) presence of stenosis at the planned embolization site of the fistula pathway, and (3) 1 opening to the right ventricle. Furthermore, by selecting the common carotid artery as the approach site, percutaneous treatment of the giant coronary artery fistula was successful in the neonatal period.
Coronary artery fistula is rarely reported in the fetal period [5,7,15–17], and in many of these the neonates developed early symptoms of congenital heart failure shortly after birth. In our case, congestive heart failure and cardiac enlargement were observed in the early neonatal period, as in these reports. This may have been related to a decrease in right ventricular systolic pressure due to decreased pulmonary vascular resistance after birth. In principle, early closure is the treatment of choice for large coronary artery fistula; fetal diagnosis will allow careful follow-up and treatment through the perinatal period.
Conclusions
Transcatheter occlusion of the giant coronary artery fistula using a self-expandable device was feasible even in a neonate whose body weight was 2.6 kg. Complete elimination of shunting was not necessary to relieve life-threatening congestive heart failure associated with the fistula. Treatment strategies for a such case need to be developed from multiple perspectives.
Figures
References:
1.. Vitarelli A, De Curtis G, Conde Y, Assessment of congenital coronary artery fistulas by transesophageal color Doppler echocardiography: Am J Med, 2002; 113(2); 127-33
2.. Mottin B, Baruteau A, Boudjemline Y, Transcatheter closure of coronary artery fistulas in infants and children: A French multicenter study: Catheter Cardiovasc Interv, 2016; 87(3); 411-18
3.. Song G, Zhang J, Ren W, Pediatric coronary artery fistula: Echocardiographic case reports and literature review of treatment strategy: Springerplus, 2016; 5(1); 1583
4.. El-Sabawi B, Al-Hijji MA, Eleid MF, Transcatheter closure of coronary artery fistula: A 21-year experience: Catheter Cardiovasc Interv, 2020; 96(2); 311-19
5.. Sharland GK, Konta L, Qureshi SA, Prenatal diagnosis of isolated coronary artery fistulas: Progression and outcome in five cases: Cardiol Young, 2016; 26(5); 915-20
6.. Aggarwal V, Mulukutla V, Qureshi AM, Justino H, Congenital coronary artery fistula: Presentation in the neonatal period and transcatheter closure: Congenit Heart Dis, 2018; 13(5); 782-87
7.. Buccheri D, Chirco PR, Geraci S, Coronary artery fistulae: Anatomy, diagnosis and management strategies: Heart Lung Circ, 2018; 27(8); 940-51
8.. Wang X, Pang C, Liu X, Congenital coronary artery fistula in pediatric patients: Transcatheter versus surgical closure: BMC Cardiovasc Disord, 2020; 20(1); 484
9.. Warnes CA, Williams RG, Bashore TM, ACC/AHA 2008 guidelines for the management of adults with congenital heart disease: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Develop Guidelines on the Management of Adults with Congenital Heart Disease). Developed in Collaboration with the American Society of Echocardiography, Heart Rhythm Society, International Society for Adult Congenital Heart Disease, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons: J Am Coll Cardiol, 2008; 52(23); e143-e263
10.. Jayaram N, Spertus JA, Kennedy KF, Modeling major adverse outcomes of pediatric and adult patients with congenital heart disease undergoing cardiac catheterization: Observations from the NCDR IMPACT Registry (National Cardiovascular Data Registry Improving Pediatric and Adult Congenital Treatment): Circulation, 2017; 136(21); 2009-19
11.. Kou L, Wang Q, Long WA, Tang F, Li L, Emerging predictors of femoral artery occlusion after pediatric cardiac catheterization: Sci Rep, 2020; 10(1); 14001
12.. Mehta R, Lee KJ, Chaturvedi R, Benson L, Complications of pediatric cardiac catheterization: A review in the current era: Catheter Cardiovasc Interv, 2008; 72(2); 278-85
13.. Mobley MM, Stroup RE, Kaine SF, Comparative risk of cardiac catheterisations performed on low birth weight neonates: Cardiol Young, 2013; 23(5); 722-26
14.. Holzer RJ, Gauvreau K, Kreutzer J, Relationship between procedural adverse events associated with cardiac catheterization for congenital heart disease and operator factors: Results of a multi-institutional registry (C3PO): Catheter Cardiovasc Interv, 2013; 82(3); 463-73
15.. Daniel M, Mavroudis C, Preminger T, Prenatal diagnosis and neonatal surgical management of a giant proximal right coronary artery to right ventricular fistula: World J Pediatr Congenit Heart Surg, 2010; 1(2); 243-48
16.. Nagiub M, Mahadin D, Gowda S, Aggarwal S, Prenatal diagnosis of coronary artery fistula: A case report and review of literature: AJP Rep, 2014; 4(2); e83-86
17.. Oztunc F, Gokalp S, Yuksel MA, Prenatal diagnosis of left coronary artery to right ventricle fistula: J Clin Ultrasound, 2015; 43(2); 129-31
Figures
In Press
14 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942824
14 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943118
14 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942826
14 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942770
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250