05 December 2021: Articles 
Efficacy of Systemic Acyclovir as Adjuvant Therapy for Oral Lichen Planus
Unusual setting of medical care
Dewi Zakiawati12ABCDEF*, Muhammad Al Farisyi1ABCDF, Tenny Setiani Dewi2ACDEFDOI: 10.12659/AJCR.934554
Am J Case Rep 2021; 22:e934554
Abstract
BACKGROUND: Oral lichen planus (OLP) is a chronic inflammatory disease involving the oral mucosa, associated with the T-cell activity that mediates an autoimmune condition, with various predisposing factors, such as herpes simplex virus (HSV). The first-line treatment is topical corticosteroids. However, additional therapy can be given according to the underlying factors. This report assessed the efficacy of oral acyclovir as adjuvant therapy in the management of OLP.
CASE REPORT: A 73-year-old man came to our unit reporting he had recurring sores on the tongue for the past 10 years. The tongue was painful and there was taste impairment. Intraoral examination showed erosion and erythematous areas surrounded by white net-like plaques on the tongue and buccal mucosa, as well as depapillation on 2/3 dorsal anterior of the tongue. The diagnosis of reticular and erosive OLP was determined based on clinical features. The patient was prescribed topical corticosteroids, multivitamins, and mouthwash containing chlorine dioxide. Supporting examinations were performed to rule out systemic predisposing factors. The patient was referred for anti-HSV-1 IgG testing, and it was reactive (34.8 U/mL). Thus, oral acyclovir was prescribed. After 2 weeks of antiviral treatment, the tongue pain and altered taste were resolved, and the clinical features showed significant improvement.
CONCLUSIONS: Management of OLP requires a comprehensive approach. OLP symptoms can be relieved if treatment is not only limited to reducing the inflammation but also seeks to remedy other comorbidities, in this case, administration of an antiviral agent to resolve the HSV-1 involvement.
Keywords: acyclovir, Adjuvants, Pharmaceutic, Lichen Planus, Oral, Herpes Simplex, Dentistry, Pathology, Oral, Combined Modality Therapy, Humans, Immunotherapy, Male, Mouth Mucosa
Background
Lichen planus (LP) came from the Greek word leichen, which means moss, and planus means flat [1]. It was first reported by Erasmus Wilson in 1869, and in 1895 Thieberg was the first to identify the oral lesion from an LP patient [2]. LP is a chronic mucocutaneous inflammatory disease that involves the skin, oral and genital mucosa, hair follicles of the scalp, and fingernails [3]. Oral lichen planus (OLP) is a lichen planus involving the oral mucosa and is associated with the T-cell activity that mediates an autoimmune condition [4,5]. OLP can co-occur with LP or can precede LP. Around 1–2% of the world population has OLP [5]. It mostly occurs in females (approximately 77%) aged 30–80 years old, with no race differences [2,6].
People who suffer from OLP may feel pain, burning, but can also be asymptomatic [2,7]. The predisposing factors are varied, such as stress, flavoring agents, systemic medications (beta-blockers, methyldopa, penicillamine, quinidine, and quinine), dental restorative materials (amalgam, composite resin, cobalt, and gold), genetics, food allergy, trauma, systemic conditions (autoimmune, immunodeficiency, inflammatory bowel disease, diabetes mellitus, hypertension, malignant neoplasm), unhealthy lifestyle (smoking, alcohol), and viral involvement with herpes simplex virus 1 (HSV-1), Epstein-Barr virus, cytomegalovirus, human herpesvirus 6 and 7, human papillomavirus (HPV), hepatitis C virus (HCV), and
OLP has 6 different clinical manifestations: reticular, plaque, erythematous/atrophic, ulcerative/erosive, bullous, and papular lesions [1,9,10]. The diagnosis of OLP can be determined by its characteristic clinical feature, commonly known as Whickham’s striae, which is a net-like white lesion [6]. The lesion appears bilaterally, mostly located in the buccal mucosa, tongue, lips, gingivae, palate, and floor of the mouth [4]. Another way to diagnose OLP is from a biopsy with immunofluorescence that shows a band-like appearance of the epithelial cells [6]. Nevertheless, wherever Whickham’s striae are visible bilaterally, this alone is sufficient to diagnose OLP [8,11].
The principle of OLP management is to suppress the activity of T cells with topical corticosteroids [12]. However, due to its various predisposing factors, additional therapy can be given according to the underlying condition. Some studies suggested that HSV-1 infection can predispose to development of OLP [2,13,14]. Therefore, acyclovir administration is a rational consideration. This report assessed the efficacy of an antiviral agent as adjuvant therapy in the management of OLP.
Case Report
A 73-year-old retired man came to the Oral Medicine Unit in Dr Hasan Sadikin General Hospital reporting painful recurring canker sores on his tongue followed by impaired taste in the last 10 years, which became worse in the past year. He has been smoking since a teenager, consumed herbal drinks, ate spicy food, and sometimes stayed up late. However, he denied having a history of diabetes mellitus, had hypertension and took captopril (without prescription) almost daily.
We found no extraoral lesions, while intraoral examination showed erosion and erythematous areas surrounded by the white net-like plaques, known as Wickham’s striae, on the dorsal and lateral sides of the tongue and the right and left sides of the buccal mucosa (Figure 1). Additionally, we found a depapillation on the 2/3 dorsal anterior part of the tongue, and the consistency of the tongue was quite rigid on palpation. The patient had poor oral hygiene and brown stains were present on all teeth due to smoking. Based on the anamnesis, as well as characteristics of Wickham’s striae on the lesions, the diagnosis of reticular and erosive OLP was made.
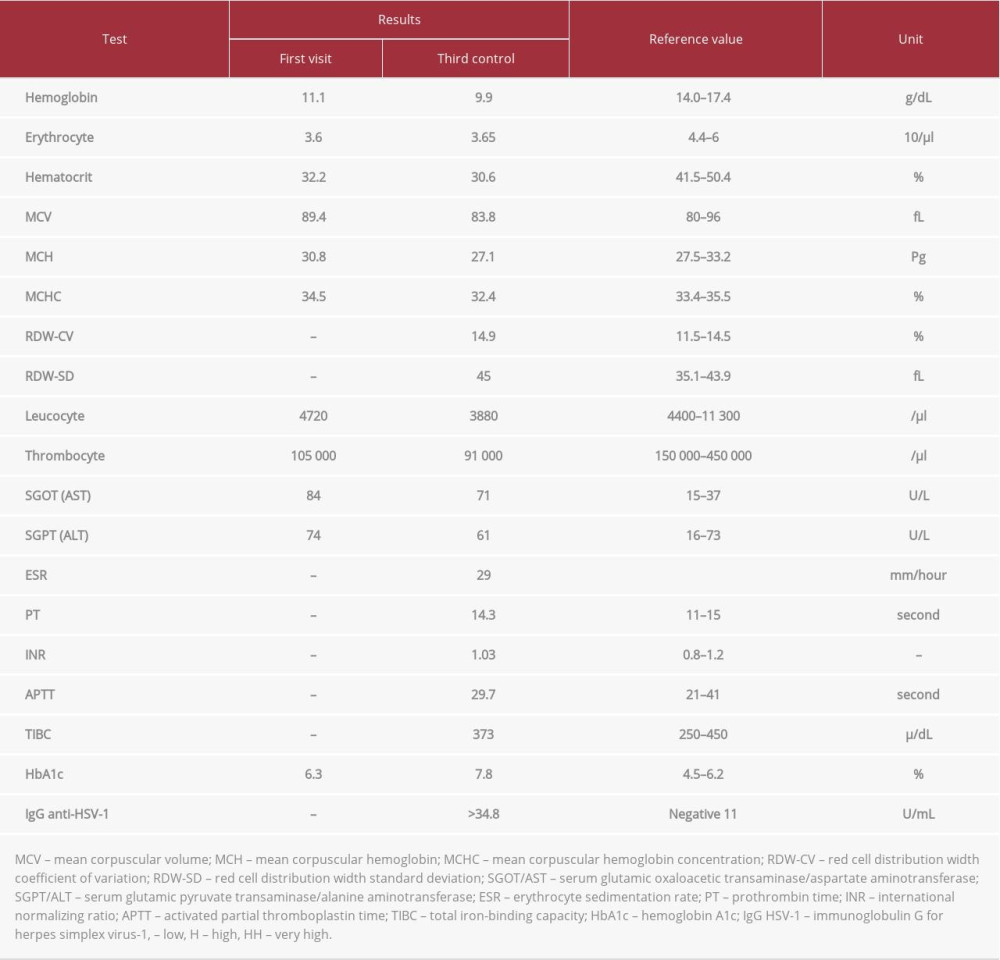
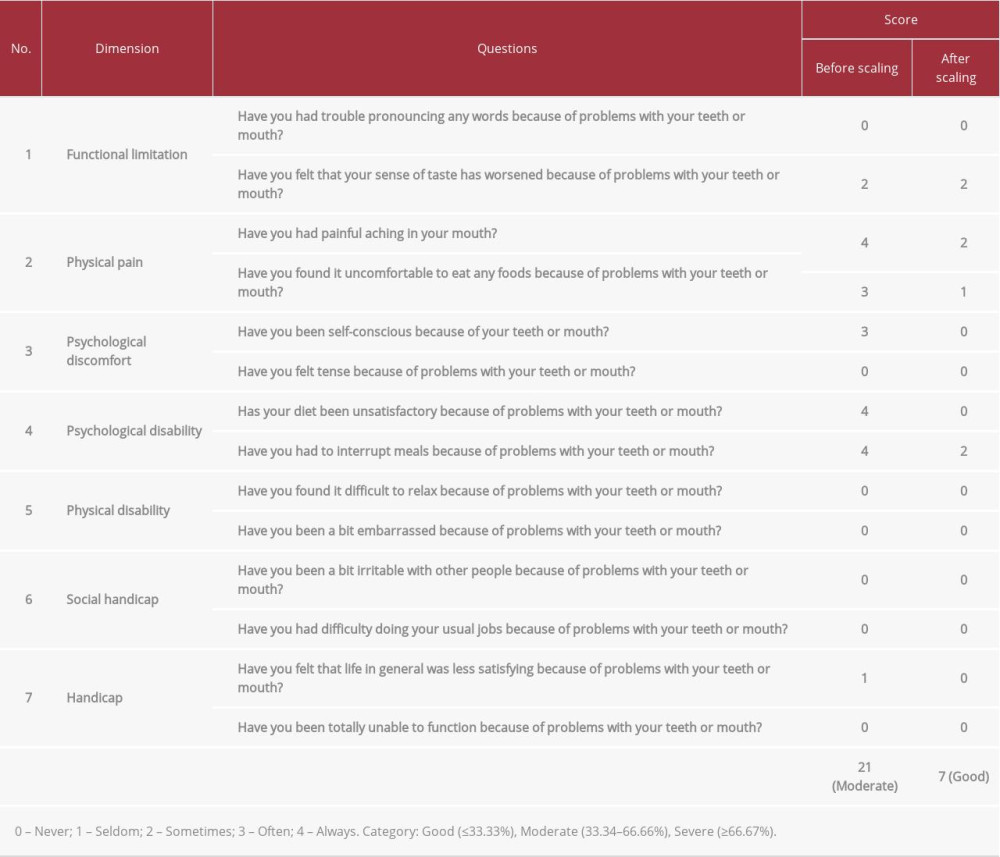
We performed 3 tests: serological examination, the Oral Health Impact Profile (OHIP-14) questionnaire, and the Depression Anxiety Stress Scale (DASS-42) questionnaire. The complete blood count showed low levels of hemoglobin, erythrocytes, hematocrit, and thrombocytes (Table 1). The liver function (serum glutamic oxaloacetic transaminase [SGOT] and serum glutamic pyruvic transaminase [SGPT]) were high. Moreover, the percentage of hemoglobin A1c (HbA1c) was slightly high (6.3%), indicating an increase in glucose level. The OHIP-14 questionnaire was used to assess how far the oral condition affected his well-being. This questionnaire is a reliable and valid tool to assess the oral health-related quality of life in various oral diseases, including OLP patients, although it was not developed especially for OLP conditions [15]. It consists of 14 questions (previously 49 questions, created by Slade and Spencer in 1994, and simplified by Slade in 1997) grouped into 7 dimensions, which assess the functional, social, and psychological effects of oral conditions in a patient’s life, as well as the dental treatment needs [16] social status, household management, daily habits, and local factors. The differences in the oral health status possibly occur in between countries, different regions, and topographical areas frequently and indirectly contributing to oral health status. The objective is to evaluate the difference of Oral Health-Related Quality of Life (OHRQoL). The test showed an improvement in patient condition before and after scaling, from moderate to good (Table 2). Lastly, to observe whether there is psychological involvement in the presence of OLP, the DASS-42 questionnaire was administered. The Depression Anxiety Stress Scale was first developed by Lovibond in 1995, consisting of 42 items (the 21-item version is also available for efficiency), divided into 3 dimensions: depression (dysphoria, hopelessness, lack of energy, and anhedonia), anxiety (irritability, agitation, difficulty relaxing, and impatience), and stress (persistent tension, a low threshold of becoming upset or frustrated, and a tendency to overreact to stressful events) [17]. Each item is scored from 0 (did not apply) to 3 (most of the time) according to what the patient has experienced in the past week, and the total score is classified as normal, mild, moderate, severe, or extremely severe. The DASS-42 result in our patient was normal to mild.
The patient was prescribed 0.5 mg dexamethasone mouth rinse (off-label drug, PT. Kimia Farma, Bandung, Indonesia), 1 mg of folic acid (PT Marin Liza Farmasi, Bandung, Indonesia), 0.1 mg vitamin B12 (PT. Kimia Farma, Bandung, Indonesia), and mouth-wash containing chlorine dioxide (Oxyfresh®, Oxyfresh Corp., Idaho, USA). We also instructed him to quit smoking, stop eating spicy food, get enough sleep, and manage stress. He was referred to the periodontology unit to remove plaque, calculus, and stains, and to the internal medicine unit to assess the glucose level and control his hypertension.
On the first and second months of control, the patient underwent scaling and quit smoking. He gradually felt better and the clinical features showed less erythema. We tapered the dexamethasone and combined it with triamcinolone acetonide in orabase. Unfortunately, the condition was flare-up in the third month. The patient admitted that he sometimes felt un-well, dizzy, and fatigued. Aside from the persisted intraoral conditions, we found a crusted ulcer on his left upper lips around the area of teeth 23–24 (Figure 2). Afterwards, serological examinations were redone to check previous systemic predisposing factors (diabetes mellitus and anemia), preparation for biopsy, and the possibility of HSV-1 infection. The anti-HSV-1 IgG was more than 3 times above normal, reaching >34.8 U/mL (Table 1). He was prescribed 200 mg acyclovir 5 times a day, and after 2 weeks of administration, the patient admitted that he felt almost no pain on his tongue and cheeks, and after years, he can taste food and drinks better.
The intraoral condition also showed improvement. The erosion and erythema on the dorsal and lateral of the tongue and also on the right buccal mucosa were nearly resolved, while the left buccal mucosa and ulcer on the lips were completely healed (Figure 3). The tongue was mild on palpation. After the last control, the COVID-19 pandemic started in Indonesia, which prevented follow-up and postponed the plan for biopsy. However, we continued communication online, and 1 week after the last visit, the patient told us that his condition was getting better each day. He maintains oral hygiene and controls diet (low sugar and carbs, also high iron) as per the instructions.
Discussion
Treating OLP patients is rather challenging due to the unclear etiopathogenesis and multifactorial agents [9,18]. Different people will have their own causative factors. Therefore, a dentist is required to make a holistic investigation to find the agents causing OLP in each patient. Our patient presented some factors that we suspected contributed to the presence of his condition, such as stress, high blood sugar and hypertension, smoking, and also HSV-1 infection. Some studies have mentioned stress as one of the precipitating factors, but the mechanism is unclear [6,8]. We consider stress might also exacerbate the patient’s condition when he said that the symptoms had started 10 years ago, quite close to the time of his retirement as a government employee when he was 60 years old. The pain was also worsened in the past year since his wife passed away. The results of the DASS questionnaire also suggested the role of stress. The result showed that he did not have depression or anxiety, but did experience mild stress. Therefore, we only suggested getting enough rest and do some activities to occupy himself and ease the grief.
The patient had a history of high blood pressure, and although he did not realize it, the laboratory findings showed an elevated HbA1c, SGOT, and SGPT concentration (presumably caused by the routine captopril intake, and long-term herbal drinks consumption). A diabetic patient with a history of hypertension can develop OLP, also called Grinspan’s syndrome [5,11]. Nevertheless, the association between the 3 entities is unclear. A meta-analysis study by Garlapati, Naik, and Sharma in 2017 found there was no association between OLP, diabetes mellitus, and vascular hypertension [5].
Topical corticosteroid is the drug of choice for OLP [11,19]. It can also be given systemically when the lesion is widespread [11]. The lesion in our patient was painful, erosive, and localized on the tongue and buccal mucosa. The Guidelines for the Management of Oral Lichen Planus by the British Society for Oral Medicine, as well as a report from the World Workshop on Oral Medicine 2007, still consider corticosteroid as the first-line therapy, especially for symptomatic atrophic/ulcerative/erosive types [12,20]. Indeed, medium- to high-potency corticosteroid (Orabase or mouthwash) can be administered with some considerations, such as the severity and location of the lesion [12,19], older age, and comorbid conditions [21]. Long-term corticosteroid consumptions will promote hyper-glycemia, leads to increased difficulty with glycemic control, and can cause fatty liver; thus, it must be carefully administered in diabetic patients and people with liver enzyme disorders [21,22]. Based on this rationale, dexamethasone mouth-wash in combination with topical triamcinolone was prescribed due to the presence of his systemic conditions.
We prescribed oral acyclovir as an adjuvant therapy to our patient based on the clinical outcome, level of HSV-1 IgG, and considering evidence from previous reports. Research has investigated the contribution of viral agents, including HSV-1 in the pathogenesis of LP and OLP. A case-control study of 60 cutaneous classic LP subjects confirmed the role of HHV-7 in the pathogenesis of LP [23]. On the contrary, research done by Ali in 2014 did not show a significant correlation between HSV-1 and OLP by immunofluorescent examination [13]. A similar study done in the same year by Park and Choi also failed to detect HSV-1 and -2 in OLP specimens by PCR test [2]. Interestingly, the level of HSV-1 and HSV-2 IgG titer increased in all 30 subjects (3–10 times above the normal titer), and 61.5% of subjects who were treated using oral acyclovir showed clinical improvement. A case report in 2016 supports that oral acyclovir administration is effective for lichen planus [14]. A recent study in Pakistan found 76.7% of eruptive LP patients had a satisfactory response to acyclovir [24]. Although the connection between OLP and HSV-1 remains unclear, the use of oral acyclovir in OLP patients has been shown to be beneficial. Aside from antiviral agents, some unexplored variables, such as probiotics [25] and photobiomodulation [26], should be considered in future clinical trials for OLP patients. This approach demonstrated promising results by modifying clinical and microbiological parameters in the oral environment that may also affect the response to OLP.
The World Health Organization (WHO) has designated OLP as an oral premalignant condition since 2005 [6]. Factors that may increase the risk of its malignant transformation are poor nutrition, tobacco and alcohol use, as well as HCV infection [11]. Our patient had been smoking since he was young. After being given information regarding the harmful effect of tobacco use on his oral health, the patient was willing to reduce his smoking and finally decided to quit completely. We planned a biopsy to further assess any unfavorable conditions, but the agenda was re-evaluated after reviewing the improvement in the signs and symptoms and considering the patient’s age and systemic diseases that make him vulnerable to COVID-19.
Conclusions
OLP is a complex disease because it has multifactorial predis-posing factors. The management of OLP requires careful attention and a comprehensive approach. Although it may take time to resolve completely, OLP symptoms can be relieved by reducing inflammation and managing possible underlying factors. In this case, where the HSV-1 IgG was reactive, the administration of oral acyclovir was effective as adjuvant therapy.
Figures
References:
1.. Gupta S, Jawanda MK, Oral lichen planus: An update on etiology, pathogenesis, clinical presentation, diagnosis and management: Indian J Dermatol, 2015; 60(3); 222-29
2.. Park S-Y, Choi EH, Relevance of herpes simplex virus infection to oral lichen planus: Univers J Med Sci, 2014; 2(3); 25-30
3.. : Oral lichen planus [Internet], 2019; 1-5, London, British Association of Dermatologists Available from: www.bad.org.uk/leaflets
4.. Greenberg MS, Glick M: Burket’s oral medicine and diagnosis 12th edition, 2008; 230-60
5.. Garlapati K, Naik V, Sharma G, The Grinspan syndrome: “fact” or “fiction” – a meta analysis research: J Pierre Fauchard Acad (India Sect), 2017; 31(2–4); 84-88
6.. Cheng YSL, Gould A, Kurago Z, Diagnosis of oral lichen planus: A position paper of the american academy of oral and maxillofacial pathology: Oral Surg Oral Med Oral Pathol Oral Radiol, 2016; 122(3); 322-54
7.. Payeras MR, Cherubini K, Figueiredo MA, Salum FG, Oral lichen planus: Focus on etiopathogenesis: Arch Oral Biol, 2013; 58(9); 1057-69
8.. Carrozzo M, Understanding the pathobiology of oral lichen planus: Curr Oral Heal Rep, 2014; 1; 173-79
9.. Ma J, Zhang J, Zhang Y, Lv T, Liu J, The magnitude of the association between human papillomavirus and oral lichen planus: A meta-analysis: PLoS One, 2016; 11(8); 1-12
10.. Gaurav , Naik V, Sodhi A, Oral erosive lichen planus – a case report with a highlight on etiopathogeneses and immunomodulatory effect of tacrolimus in management of OELP: MOJ Clin Med Case Rep, 2016; 5(2); 209-12
11.. Kökten N, Uzun L, Karadağ AS, Grinspan’s syndrome: A rare case with malignant transformation: Case Rep Otolaryngol, 2018; 2018; 9427650
12.. Lavanya N, Jayanthi P, Rao U, Ranganathan K, Oral lichen planus: An update on pathogenesis and treatment: J Oral Maxillofac Pathol, 2011; 15(2); 127-32
13.. Ali , Muthanna K, Immunofluorescence assessment of herpes simplex virus type 1 in oral lichen planus: J Baghdad Coll Dent, 2014; 26(1); 103-7
14.. Abdelmaksoud A, Acyclovir for treatment of lichen planus: Wiley Dermatologic Ther February, 2017; 3-5
15.. Yuwanati M, Gondivkar S, Sarode SC, Impact of oral lichen planus on oral health-related quality of life: A systematic review and meta-analysis: Clin Pract, 2021; 11(2); 272-86
16.. Husain FA, Tatengkeng F, Oral health-related quality of life appraised by OHIP-14 between urban and rural areas in Kutai Kartanegara Regency, Indonesia: Pilot pathfinder survey: Open Dent J, 2017; 11(1); 557-64
17.. Manczyk B, Gołda J, Biniak A, Evaluation of depression, anxiety and stress levels in patients with oral lichen planus: J Oral Sci, 2019; 61(3); 391-97
18.. Mester A, Lucaciu O, Ciobanu L, Clinical features and management of oral lichen planus (OLP) with emphasis on the management of hepatitis c virus (HCV)-related OLP: Bosn J Basic Med Sci, 2018; 18(3); 217-23
19.. Johnson L, Perschbacher K, Leong I, Bradley G, Oral manifestations of immunologically mediated diseases: Atlas Oral Maxillofac Surg Clin North Am, 2017; 25(2); 171-85
20.. , Guidelines for the management of oral lichen planus in secondary care: The British Society for Oral Medicine, 2010; 1-9
21.. Yasir M, Amandeep G, Pankaj B, Sindharth S: Corticosteroid adverse effects [Internet], 2021; 1-74, Maryland, Statpearls publishing LLC Available from: https://www.ncbi.nlm.nih.gov/books/NBK531462/
22.. Ganda KM: Dentist’s guide to medical conditions and complications, 2008, Blackwell, Munksgaard
23.. Nahidi Y, Tayyebi Meibodi N, Ghazvini K, Esmaily H, Association of classic lichen planus with human herpesvirus-7 infection: Int J Dermatol, 2017; 56(1); 49-53
24.. Akhtar A, Fatima N, Sattar F, Treatment of eruptive lichen planus with oral acyclovir: J Pakistan Assoc Dermatologists, 2020; 30(1); 53-57
25.. Butera A, Gallo S, Maiorani C, Probiotic alternative to chlorhexidine in periodontal therapy: Evaluation of clinical and microbiological parameters: Microorganisms, 2021; 9(1); 69
26.. Ferri EP, Cunha KRL, Abboud CS, Photobiomodulation is effective in oral lichen planus: A randomized, controlled, double-blind study: Oral Dis, 2021; 27(5); 1205-16
Figures
In Press
06 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942937
12 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943244
13 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943275
13 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943411
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250