13 November 2020: Articles 
Contrast-Induced Transient Neurological Symptoms Following Percutaneous Coronary Intervention: A Case Report
Challenging differential diagnosis, Unusual or unexpected effect of treatment, Diagnostic / therapeutic accidents, Unexpected drug reaction, Rare disease, Clinical situation which can not be reproduced for ethical reasons
Aishah Albakr1ABCDEF*, Noman Ishaque1EF, Danah Aljaafari1F, Sabah N. Sairafi1EDOI: 10.12659/AJCR.926956
Am J Case Rep 2020; 21:e926956
Abstract
BACKGROUND: Transient neurological symptoms after a percutaneous coronary intervention (PCI) are not uncommon manifestations. In clinical practice, the development of these symptoms might be a warning sign for PCI-related ischemic or hemorrhagic stroke. However, there is a reported risk of contrast-induced neurological injury (CINI) after PCI, which results in a broad spectrum of transient and benign neurological symptoms. Advanced age, renal disease, diabetes, hypertension, and brain parenchymal lesions are risk factors for CINI.
CASE REPORT: A 78-year-old man with diabetes and impaired renal function developed left-sided hemiparesis and dysarthria within one hour of PCI. Non-contrast CT head showed hyperdense lesions in both frontal lobes, while the susceptibility-weighted sequence of magnetic resonance imaging (SWI-MRI) excludes hemorrhage. Hemodialysis had to be started for fast contrast clearance, and he had recovered completely within 24 hours.
CONCLUSIONS: This case demonstrates that CINI is an important differential diagnosis that cardiologists and neurologists must be familiar with, especially for high-risk patients. The prognosis is good; whether an appropriate contrast’s dose or type for PCI or a need for early hemodialysis to avoid CINI in those patients is unclear.
Keywords: Cerebral Hemorrhage, Contrast Media, Coronary Angiography, Extravasation of Diagnostic and Therapeutic Materials, Stroke, Magnetic Resonance Imaging, percutaneous coronary intervention, Risk Factors
Background
Cardiac catheterization is currently performed frequently, leading to increased risk of associated neurologic complications [1,2]. The frequency of neurologic complications after cardiac catheterization has been reported to range from 0.03% to 0.3% for diagnostic procedures and from 0.3% to 0.4% for therapeutic procedures [1–3]. CINI is a rare complication of coronary angiography, with few reported cases [4]. Clinical symptoms may vary from an altered level of consciousness and cortical blindness to seizures and focal neurological symptoms [4]. Neuroimaging is an important tool that has helped physicians to diagnose contrast retention and to exclude ischemic or hemorrhagic complications of PCI [5]. However, in some cases, it can pose a diagnostic dilemma and thus complicate the decision about the use of antithrombotics following PCI. For example, post-procedural intracerebral hemorrhage (ICH) may necessitate holding anti-platelets, with increased risk for stent thrombosis [2], while post-PCI ischemic stroke may require thrombolysis use with increased risk of hemorrhages, especially in high-risk patients [2]. As CINI can resemble stroke clinically or radiologically, further neuroimaging studies, including dual-energy CT scan or brain MRI, may be necessary to differentiate lesions as being related to contrast
Case Report
We present the case of a 78-year-old right-handed man with a history of uncontrolled diabetes, hypertension, and end-stage renal disease ESRD, who was on peritoneal dialysis and a history of right middle cerebral artery (MCA) stroke 6 months ago, who presented to the Emergency Department with a complaint of chest pain. His electrocardiogram demonstrated a non-ST elevation myocardial infarction. The coronary angiogram was performed via right radial artery access, followed by PCI with a drug-eluting stent deployed into the circumflex and right coronary artery (RCA). Around 190 mL of Iohexol (Omnipaque 350) was used during the procedure. He also had received 7500 IU heparin, 300 mg clopidogrel, and 100 mg aspirin. The procedure lasted for 55 min, with stable blood pressure and excellent angiographic results. One hour later, the patient developed left-sided weakness and dysarthria. The stroke code was activated by the Cardiology team. On examination, his vital signs were stable. He had moderate dysarthria, mild left upper motor neuron facial palsy, and the motor power in the left arm and left leg was 3 out of 5 on the Medical Research Council scale, along with decreased sensation on the left side of the body. Plantar response was extensor bilaterally. The National Institute of Health stroke scale score was 7. His blood glucose was 197 mg/dl. A head CT showed hyperdense lesions in both frontal lobes (Figure 1). A diagnosis of ICH was considered; therefore, an MRI head was done immediately to differentiate contrast extravasation from bleeding. SWI-MRI did not show any signal drop-out in areas that showed hyperdense lesions on head CT (Figures 2, 3), and DWI-MRI did not show restricted diffusion. Aspirin and clopidogrel were resumed. Hemodialysis had to be started for quick contrast removal, and his symptoms had improved completely within 24 h. Laboratory investigations excluded infection but showed a raised hemoglobin A1c of 10.3 and creatinine of 5.6 mg/dl. His echocardiogram demonstrated moderate global hypokinesia, with moderate left ventricular systolic dysfunction (EF 33%). Supportive care was maintained for 4 days, and he was discharged with complete recovery. His CT head was repeated after 72 h, showing complete resolution of the hyperdense lesions.
Discussion
This case demonstrates that CINI can be a possible cause of new neurological symptoms following PCI, especially in an elderly diabetic person with impaired renal function. This may have an impact on the clinical decision-making process in situations in which differentiating contrast retention from stroke is crucial and might be even a life-saving. In our patient, the brain MRI was performed to exclude ICH, and antiplatelet was thus resumed to keep stent patency. Consistent with the previous report, this patient experienced complete recovery within 24 h.
The mechanisms by which contrast enhancement occurs following coronary angiography remain largely obscure. Many hypotheses have been proposed, including direct disruption of the blood-brain barrier (BBB) induced by the chemical or ionic properties of the contrast material [9,10]. The hyper-osmolarity changes, hyperviscosity, and vasodilator characters of the contrast agents might create high intraluminal pressure and thus a greater BBB disruption [9,10]. In the present case, the contrast enhancement in the right frontal lobe may be partially explained by the presence of chronic infarction in areas of extravasation, causing BBB rupture. However, the patient also had contrast retention of the left frontal lobe. Certain well-recognized clinical factors [11] have been attributed to this finding in our patient. First, clearance of contrast material was probably delayed because of ESRD. Second, uncontrolled diabetes may contribute to a higher vascular permeability and BBB disruption. Third, advanced age and poor cardiac function may be an additional factor. Hypertension is a well-known factor for CINI as it can also affect BBB [11]; however, as the patient’s blood pressure readings were well-controlled, it does not seem to play a large contributory role here.
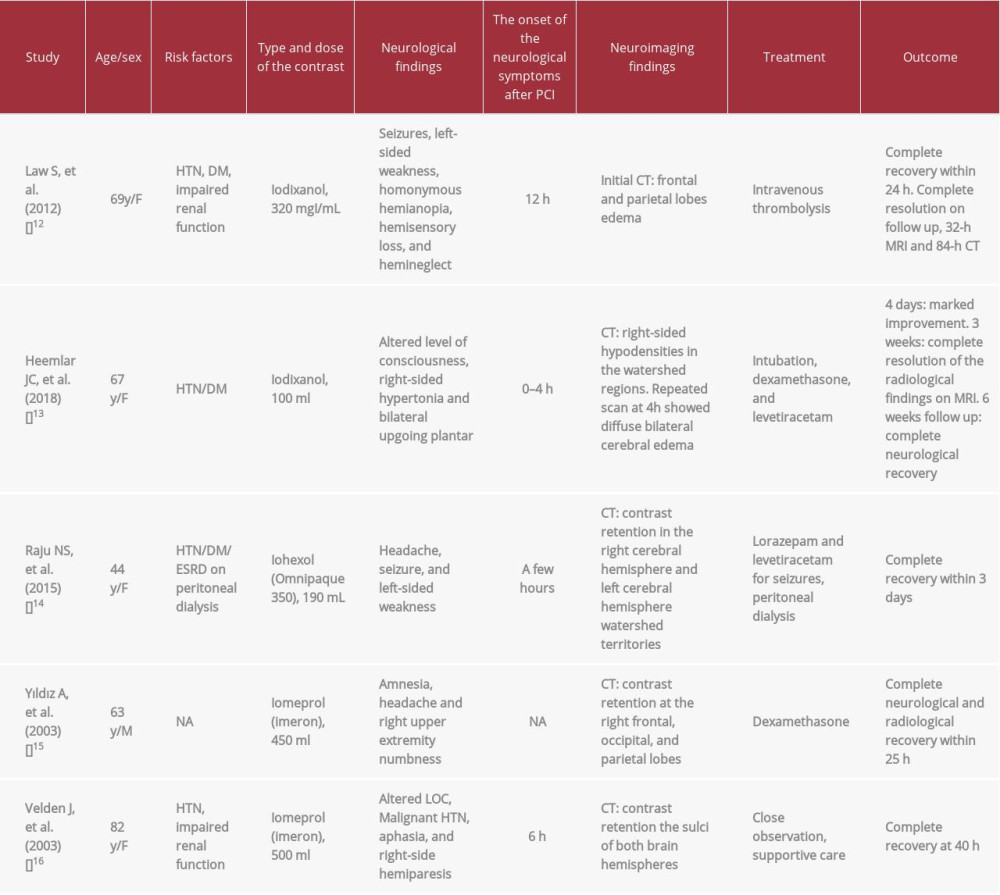
A recent systematic review of the literature involving 75 cases of CINI in the context of coronary angiography showed that reversible cortical blindness is the most commonly reported symptom, followed by changes in mental status. Focal neurological symptoms are uncommon and have been reported in only 5 cases [12–16]. Neurological events usually develop within 2 to 12 h of coronary angiography and mostly improve in 24 to 72 h [4]. Table 1 summarizes the reported cases in the literature of transient focal neurological symptoms following PCI. The clinical and radiological findings in our case seem to be similar to the previous reports [12–16]. There is no existing recommendation for contrast type or dose used for a coronary angiogram to avoid CINI. In our case, the patient had ESRD and 120 ml of Iohexol was administered. It is hypothetically correct that Iohexol has a low risk for CINI as it is a nonionic contrast agent with a relatively low or iso-osmolarity feature. Kariyanna et al. stated that cerebral contrast retention has been reported with all types of contrast agents, regardless of their osmolality or ionic features, there is no clear association between the contrast dose and CINI, and most of the events occur with administration of 100 ml or more of the contrast agent, similar to our case [4].
Given the well-recognized neurological complications of PCI [2], it is crucial to differentiate between stroke and contrast extravasation. IV thrombolysis (IVT), which is the standard acute stroke therapy, are relatively safe for non-stroke patients (i.e., those with stroke-mimics diagnoses); however, there remains a concern for the IVT-related hemorrhagic complications and orolingual edema, especially in high-risk patients, including old age, recent antithrombotic use, and past stroke [17]. Law et al. reported a case of CINI treated with thrombolysis due to the presumption of stroke diagnosis [12]. Such therapy may expose the patients to unnecessary treatment for a benign and reversible condition [2]. In our case, considering the history of ischemic stroke, antithrombotic use during the PCI, and a low reported risk of CINI after PCI, the ICH diagnosis was a huge concern. As acute stent thrombosis (AST) is a dangerous complication of PCI, with a high mortality rate [18], holding antiplatelet administration was a challenging task for the neurologists and cardiologists. The difficulty in distinguishing between blood and iodine contrast on CT lies in the fact that they share similar densities [7]. Studies have reported various methods to differentiate contrast extravasation from ICH. In a study on acute stroke patients who underwent endovascular treatment, an average attenuation of less than 50 Hounsfield units was found to be sufficient to differentiate contrast extravasation from ICH [7]. Dual-energy CT scans obtained at 80 kV and 140 kV is also described as highly accurate in differentiating contrast extravasation from ICH [6]. Finally, head MRI with diffusion as well as SWI was described as an effective means to detect hemorrhage and to differentiate it from contrast in acute stroke patients who underwent thrombolytic therapy [8]. In our patient, MRI of the brain with SWI was chosen because it is fast, reliable, and easily accessible.
Overall, complete clinical and radiological recovery of CINI have been reported with supportive management, including adequate hydration and close observation. In most of the reported cases [4], as in our patient, rapid recovery occurs within days. Considering the impaired renal function and CINI, we considered hemodialysis for rapid contrast clearance. In our case, complete neurological recovery, as well as the resolving radiological finding, on follow-up CT led to the diagnosis of CINI. Further studies are required to determine the optimal contrast dose in ESRD patients, as well to determine the timing and need for hemodialysis following PCI to avoid this rare but important condition.
Conclusions
CINI is an essential differential diagnosis that must be considered in high-risk patients following PCI. This condition is benign but can pose a diagnostic dilemma. Once the diagnosis has been confirmed, supportive care is often adequate. It is unclear whether hemodialysis is essential or has an impact on outcomes that need to be investigated in future studies.
Figures
References:
1.. Tavakol M, Ashraf S, Brener SJ, Risks and complications of coronary angiography: A comprehensive review: Glob J Health Sci, 2012; 4(1); 65-93
2.. Werner N, Bauer T, Hochadel M, Incidence and clinical impact of stroke complicating percutaneous coronary intervention: Results of the Euro heart survey percutaneous coronary interventions registry: Circ Cardiovasc Interv, 2013; 6(4); 362-69
3.. Kocabay G, Karabay CY, Kalayci A, Contrast-induced neurotoxicity after coronary angiography: Herz, 2014; 39(4); 522-27
4.. Kariyanna PT, Aurora L, Jayarangaiah A, Neurotoxicity associated with radiological contrast agents used during coronary angiography: A systematic review: Am J Med Case Rep, 2020; 8(2); 60-66
5.. Ho SK, Lee JK, Lai YJ, Differentiating contrast staining after acute ischemic stroke from hemorrhagic transformation during emergency evaluation: Am J Emerg Med, 2016; 34(11); 2255.e5-6
6.. Phan CM, Yoo AJ, Hirsch JA, Differentiation of hemorrhage from iodinated contrast in different intracranial compartments using dual-energy head CT: Am J Neuroradiol, 2012; 33(6); 1088-94
7.. Dekeyzer S, Nikoubashman O, Lutin B, Distinction between contrast staining and hemorrhage after endovascular stroke treatment: One CT is not enough: J Neurointerv Surg, 2017; 9(4); 394-98
8.. Greer DM, Koroshetz WJ, Cullen S, Magnetic resonance imaging improves detection of intracerebral hemorrhage over computed tomography after intra-arterial thrombolysis: Stroke, 2004; 35(2); 491-95
9.. Sterrett PR, Bradley IM, Kitten GT, Cerebrovasculature permeability changes following experimental cerebral angiography. A light- and electron-microscopic study: J Neurol Sci, 1976; 30(2–3); 385-403
10.. Lalli AF, Contrast media reactions: Data analysis and hypothesis: Radiology, 1980; 134(1); 1-12
11.. Yu J, Dangas G, Commentary: New insights into the risk factors of contrast-induced encephalopathy: J Endovasc Ther, 2011; 18(4); 545-46
12.. Law S, Panichpisal K, Demede M, Contrast-induced neurotoxicity following cardiac catheterization: Case Rep Med, 2012; 2012; 267860
13.. Heemelaar JC, van der Hoeven NW, Muller FF, Appelman Y, Acute-onset coma after iso-osmolar iodinated contrast injection: A case report of contrast-induced encephalopathy after elective coronary angiography: Eur Heart J Case Rep, 2018; 2(4); yty132
14.. Gollol Raju NS, Joshi D, Daggubati R, Movahed A, Contrast-induced neurotoxicity following coronary angiogram with Iohexol in an end-stage renal disease patient: World J Clin Cases, 2015; 3(11); 942-45
15.. Yildiz A, Yencilek E, Apaydin FD, Transient partial amnesia complicating cardiac and peripheral arteriography with nonionic contrast medium: Eur Radiol, 2003; 13(Suppl. 4); L113-15
16.. Velden J, Milz P, Winkler F, Nonionic contrast neurotoxicity after coronary angiography mimicking subarachnoid hemorrhage: Eur Neurol, 2003; 49(4); 249-51
17.. Tsivgoulis G, Zand R, Katsanos AH, Safety of intravenous thrombolysis in stroke mimics: Prospective 5-year study and comprehensive meta-analysis: Stroke, 2015; 46; 1281-87
18.. Ge J, Yu H, Li J, Acute coronary stent thrombosis in modern era: Etiology, treatment, and prognosis: Cardiology, 2017; 137(4); 246-55
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133