14 June 2022: Articles 
Variant in the Blood of a Patient with Gastric Cancer Undergoing Tumor Profiling Tests Diagnosed as Clonal Hematopoiesis
Challenging differential diagnosis
Miki Kawai1ADEF, Yuka Iijima-Yamashita2CD, Iku Taguchi1BD, Masato Kataoka3ABE, Masashi Sanada2CDEF, Yoshiko MurakamiDOI: 10.12659/AJCR.936455
Am J Case Rep 2022; 23:e936455
Abstract
BACKGROUND: Clonal hematopoiesis is the production of a specific single clonal type of cell in the blood and is often found in cancer genomic profiling tests. When the clone carries a pathogenic variant, it may be important to differentiate between somatic or germline origin. The variant in the blood that has a lower minor allele frequency could reflect heterozygous germline origin, somatic mosaicism, and clonal hematopoiesis. It is important to evaluate suspected variants to determine the course of treatment and follow-up of the patient, depending on the patient’s medical condition and family situation.
CASE REPORT: We report a 53-year-old Japanese man with gastric cancer who underwent a cancer genomic profiling test searching for therapeutic agents. The profiling test detected a variant, TP53 c.559+2T>G minor allele frequencies of 9% (168/1865) in tumor tissue and 29.1% (58/199) in paired blood. Since the TP53 variant has the possibility of Li-Fraumeni syndrome, ancillary testing was performed using fingernails, buccal swab, and blood specimens. The genomic analysis revealed no TP53 variant in his fingernails. The patient had previously received platinum-based chemotherapies, suggesting that the variant reflected treatment-induced clonal hematopoiesis.
CONCLUSIONS: Identifying clonal hematopoiesis when performing genomic profiling tests for patients with cancer is important. Examining multiple tissues to determine whether a variant arises from clonal hematopoiesis or is of germline origin can provide more accurate genetic information and improve patient follow-up care.
Keywords: Clonal Hematopoiesis, Li-Fraumeni syndrome, Tumor Suppressor Protein p53, Genes, p53, Genetic Predisposition to Disease, Humans, Male, Middle Aged, Stomach Neoplasms
Background
The increasing use of next-generation sequencing has enabled the development of cancer treatment strategies that target certain gene profiles using effective therapeutic agents. More than 300 cancer-associated genes have been identified as actionable variants [1]. Tests of tumor tissue and paired blood show that the percentage of variants in the latter is approximately 50% in general; these are usually assumed to be of germline origin. Variants in the blood that have a lower minor allele frequency (MAF) could reflect post-zygotic mosaicism [2].
Additionally, the possibility of clonal hematopoiesis (CH), which is a skewing in blood cell clones, should be considered if the patient is undergoing cancer treatment [3]. Whether variants are heterozygous germline, somatic mosaicism, or CH will determine the patient’s treatment and/or follow-up strategy; therefore, evaluating the suspected variant is important, although the necessity of doing so varies depending on the patient’s medical condition and family situation.
In this report, we describe a patient with gastric cancer who underwent cancer genomic profile testing of both the tumor and paired blood, whereupon
Case Report
A Japanese man was diagnosed with stage IV gastric cancer with distant lymph node metastasis as his first cancer at age of 53; the pathological diagnosis was consistent with poorly-differentiated adenocarcinoma. His initial chemotherapy regimen was 8 cycles of tegafur/gimeracil/oteracil (S-1) plus cisplatin, which was followed by 3 cycles of S-1, 7 cycles of nanoparticle albumin-bound-paclitaxel plus ramucirumab, and nivolumab. After the cancer progressed, he most recently received irinotecan, trifluridine plus tipiracil hydrochloride, and capecitabine plus oxaliplatin.
At age 57 years (3 years 4 months after his initial diagnosis with gastric cancer), the patient underwent a gastric biopsy; the specimen and paired blood were subjected to a tumor genome profiling test (NCC-OncoPanel System, Sysmex Corporation, Kobe, Japan). He was found to have a variant, NM_000546.5(TP53): c.559+2T>G, with a MAF of 9% (168/1865) in the tumor and 29.1% (58/199) in the paired blood. The splice donor variant of intron 5 lead to a loss of function at the authentic splice site; this variant was deemed to be “pathogenic” according to the American College of Medical Genetics guidelines. The MAFs of the other 4 pathogenic variants detected in tumor specimens ranged from 5.2% to 52.1%, which were within the average range reported previously [4] (Table 1).
The patient did not meet the Chompret or classical criteria for Li-Fraumeni syndrome (LFS), even though gastric cancer has been associated with LFS [5,6]. The low MAF suggested the possibility of post-zygotic mosaicism; 7 of the patient’s first- and second-degree family members had cancer, but mostly when in their 70s and 80s. Moreover, his 3 offspring (aged 30, 27, and 24 years) did not have any malignancies. Hematological malignancies such as myelodysplastic syndromes and Waldenström macroglobulinemia were ruled out because his laboratory findings (including complete blood counts) were within the normal range. His history of having received platinum-based agents such as cisplatin and oxaliplatin suggested chemotherapy-induced CH. However, to clarify whether the variant was CH, a validation test using different specimens seemed to be necessary. Although another tumor specimen (biological replicate) was not available, we offered him to have a confirmation test using nail, oral swabs, and another blood specimens, considering the minimum invasiveness. Informed consent was obtained from the patient to perform molecular DNA analysis, which was also approved by the Ethics Review Board for clinical studies at the National Hospital Organization Nagoya Medical Center (No. 2014-756).
Four milliliters of peripheral blood were drawn into an EDTA-containing tube. The buccal mucosa cells were collected using Sterile DNA-Free Large Round Foam Swab. Fingernails were cut with clean clippers and collected. The genomic DNAs were extracted from the blood using the Gentra Puregine Blood Kit (Qiagen, Inc., Valencia, CA), the buccal swab using the QIAamp DNA Mini Kit (Qiagen, Inc., Valencia, CA), and fingernail using ISOHAIR (Nippon Gene, Inc., Tokyo, Japan), according to the manufacturer’s protocols, respectively. PCR direct sequencing was performed on exon 5 and its exon-intron boundaries because the variant (c.559+2T>G) was at the 5’ splice site beginning intron 5 of
The
Taken together, we assumed the variant did not indicate post-zygotic mosaicism but rather CH. The patient and 2 of his off-spring attended a genetic counseling session, in which we explained that the variant was considered as CH, unlikely to be of germline origin. The patient and his children accepted the test results and were satisfied with the explanation. The children did not wish to have genetic testing because of the additional cost and because none of them had developed cancer. We also recommended that he undergo regular blood tests for monitoring, as CH can occasionally develop into hematological malignancies such as myelodysplastic syndromes.
Discussion
Although blood DNA is thought to represent the germline, genetic cancer risk assessment after cancer profiling testing should be performed with caution, especially when assessing variants in
The
Anticancer drugs have recently been reported to be a leading cause of CH. Platinum and topoisomerase II inhibitors are associated with CH mutations in DNA damage-response genes, such as
Herein, we discussed CH as a secondary finding on cancer panel testing; however, in the near future, the assessment of
Conclusions
Genomic profiling tests can identify CH even in non-elderly patients who have received chemotherapy. Both high MAF values and massive blood infiltration into the tumor tissue can lead to erroneous interpretations under routine specimen settings. Testing of other tissue specimens in addition to tumor and blood can lead to more accurate results. A thorough assessment of CH will be helpful for providing guidance and follow-up care for patients.
Figures
References:
1.. Frampton GM, Fichtenholtz A, Otto GA, Development and validation of a clinical cancer genomic profiling test based on massively parallel DNA sequencing: Nat Biotechnol, 2013; 31; 1023-31
2.. Batalini F, Peacock EG, Stobie L, Li-Fraumeni syndrome: not a straightforward diagnosis anymore – the interpretation of pathogenic variants of low allele frequency and the differences between germline PVs, mosaicism, and clonal hematopoiesis: Breast Cancer Res, 2019; 21; 1-10
3.. Genovese G, Kähler AK, Handsaker RE, Clonal hematopoiesis and blood-cancer risk inferred from blood DNA sequence: N Engl J Med, 2014; 371; 2477-87
4.. Sunami K, Ichikawa H, Kubo T, Feasibility and utility of a panel testing for 114 cancer-associated genes in a clinical setting: A hospital-based study: Cancer Sci, 2019; 110; 1480-90
5.. Funato M, Tsunematsu Y, Yamazaki F, Characteristics of Li-Fraumeni syndrome in Japan: A review study by the special committee of JSHT: Cancer Sci, 2021; 112; 2821-34
6.. Masciari S, Dewanwala A, Stoffel EM, Gastric cancer in individuals with Li-Fraumeni syndrome: Genet Med, 2011; 13; 651-57
7.. Weitzel JN, Chao EC, Nehoray B, Somatic TP53 variants frequently confound germ-line testing results: Genet Med, 2018; 20; 809-16
8.. Weber-Lassalle K, Harter P, Hauke J, Diagnosis of Li-Fraumeni syndrome: Differentiating TP53 germline mutations from clonal hematopoiesis: Results of the observational AGO-TR1 trial: Hum Mutat, 2018; 39; 2040-46
9.. Mitchell RL, Kosche C, Burgess K, Misdiagnosis of Li-Fraumeni syndrome in a patient with clonal hematopoiesis and a somatic TP53 mutation: J Natl Compr Cancer Netw, 2018; 16; 461-66
10.. Ito M, Fujiwara Y, Kubo T, Clonal hematopoiesis from next generation sequencing of plasma from a patient with lung adenocarcinoma: A case report: Front Oncol, 2020; 10; 113
11.. Suzuki H, Aoki K, Chiba K, Mutational landscape and clonal architecture in grade II and III gliomas: Nat Genet, 2015; 47; 458-68
12.. Behjati S, Maschietto M, Williams RD, A pathogenic mosaic TP53 mutation in two germ layers detected by next generation sequencing: PLoS One, 2014; 9; e96531
13.. Bolton KL, Ptashkin RN, Gao T, Cancer therapy shapes the fitness landscape of clonal hematopoiesis: Nat Genet, 2020; 52; 1219-26
14.. Malekzadeh P, Yossef R, Cafri G, Antigen experienced T cells from peripheral blood recognize p53 neoantigens: Clin Cancer Res, 2020; 26; 1267-76
15.. Seligmann JF, Fisher DJ, Brown LC, Inhibition of WEE1 is effective in TP53- and RAS-mutant metastatic colorectal cancer: A randomized trial (FOCUS4-C) comparing adavosertib (AZD1775) with active monitoring: J Clin Oncol, 2021; 39; 3705-15
Figures
Tables
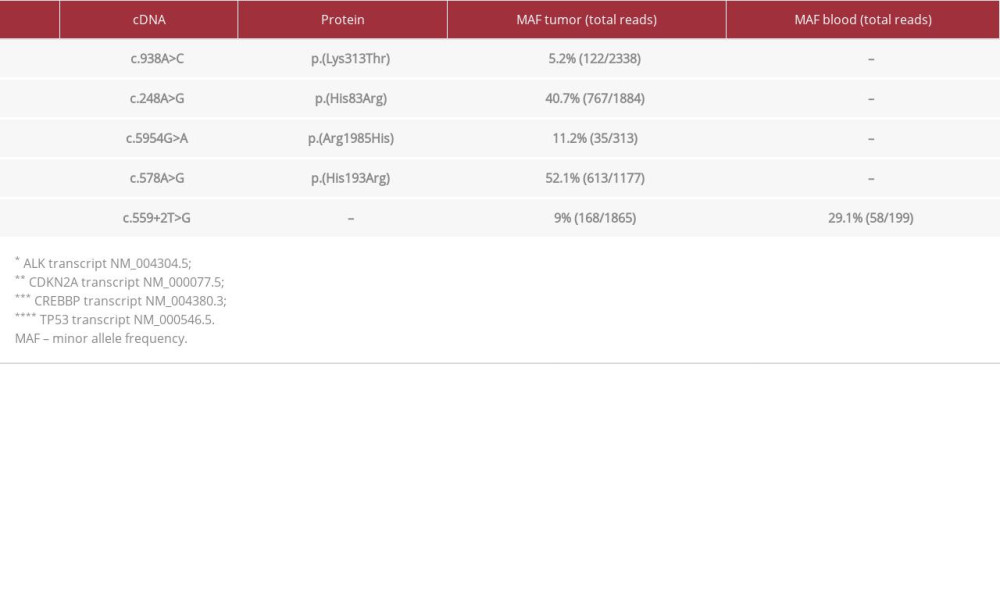 Table 1.. The MAF values are provided for each variant. The TP53: c.559+2T>G variant was present in the tumor and paired blood samples. The remaining variants were not present in the paired blood.
Table 1.. The MAF values are provided for each variant. The TP53: c.559+2T>G variant was present in the tumor and paired blood samples. The remaining variants were not present in the paired blood. Table 1.. The MAF values are provided for each variant. The TP53: c.559+2T>G variant was present in the tumor and paired blood samples. The remaining variants were not present in the paired blood.
Table 1.. The MAF values are provided for each variant. The TP53: c.559+2T>G variant was present in the tumor and paired blood samples. The remaining variants were not present in the paired blood. In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








